The Effect of Eating Behavior on Being Overweight or Obese During Preadolescence
Article information
Abstract
Objectives
Being overweight or obese is central to metabolic syndrome, and these characteristics constitute dominant risk factors for chronic diseases. Although behavioral factors, including eating habits and sedentary lifestyles, are considered to be determinants of obesity, the specific childhood factors that contribute to this condition have not been clearly defined.
Methods
The subjects consisted of 261 children aged 7-9 years who were recruited from an elementary school during October 2003. Information was obtained from their parents using a questionnaire focused on eating behaviors and lifestyle factors, additional data were also collected via anthropometric measurements and biochemical examinations, including blood tests.
Results
A total of 48 (18.4%) of the 261 children were overweight, and 34 (70.8%) had at least one other component of metabolic syndrome. Eating behaviors emerged as significant lifestyle-related risk factors for being overweight or obese. Those who engaged in overeating more than twice per week had three times the risk of being overweight (odds ratio [OR], 3.10, 95% confidence interval [CI], 1.39 to 6.92), and those who ate rapidly had three times the risk of being overweight (OR, 3.28; 95% CI, 1.68 to 6.41). Those who had fewer family meals (fewer than 2-3/month) had a nine times higher risk of being overweight than those who had family meals more frequently (at least 1/day) (OR, 9.51; 95% CI, 1.21 to 74.82).
Conclusions
This study showed that being overweight or obese during preadolescence is associated with a higher risk of metabolic syndrome and is related to unhealthy eating behaviors. Thus, weight-control strategies and healthy eating behaviors should be developed early in life to reduce the risk for metabolic syndrome.
INTRODUCTION
Obesity has become a serious global public health problem. The International Obesity Task Force reported that approximately 155 million school-aged children are overweight or obese worldwide [1]. The overall prevalence of obesity in Korea has increased consistently, moving from 5.8% in 1997 to 9.7% in 2005 [2]. Being overweight or obese is central to developing metabolic syndrome, and these characteristics constitute the dominant risk factors for chronic illnesses such as cardiovascular disease and type 2 diabetes. Additionally, being overweight or obese during childhood has long-term adverse effects on health. Thus, national attention has been focused on preventing and reducing childhood obesity, particularly in preadolescents.
Obesity is a complex problem resulting from a combination of genetic, behavioral, environmental, and socioeconomic issues [3], identification of the risk factors that are modifiable is central for obesity prevention and epidemiology. During the past few decades, behavioral changes such as the adoption of sedentary lifestyles and less healthy eating habits have contributed to obesity. Several studies have shown that a sedentary lifestyle that incorporates, for example, prolonged television viewing, physical inactivity, and unhealthy eating habits during childhood was associated with an elevated risk of developing obesity [4-6]. These findings have led to the hypothesis that the risks for obesity are not only genetic but are indeed amplified by an unhealthy lifestyle during childhood. Although behavioral factors, including eating behaviors and a sedentary lifestyle, are determinants of obesity, more specific behavioral contributors to obesity have not been clearly defined. Moreover, preventive strategies that focus on adolescents and young adults have been largely unsuccessful [4]. However, most studies have focused on adolescents or young adults, and studies of the clustering of metabolic components in preadolescent children have confirmed that the distribution of these components may provide useful information.
Therefore, we identified the effects of specific lifestyle-related risk factors, such as eating behaviors, on being overweight or obese and on the distribution of the components of metabolic syndrome in overweight and obese preadolescents.
METHODS
I. Study Subjects
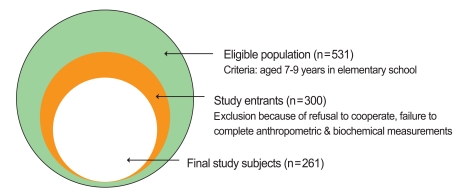
The subjects consisted of 261 Korean children aged 7-9 years who were recruited from second and third grades at an elementary school in Seoul, Republic of Korea, during October 15 and 16 of 2003. The parents or guardians of the children provided consent for their child's participation in this study. Information, including lifestyle-related data, was obtained from the parents through an eating-behavior questionnaire, data were also collected by anthropometric measurements and biochemical blood examinations (Figure 1). More detailed methods of recruiting study subjects were provided in a previously published paper [7]. This study was approved by Institutional Review Board of Ewha Womans University Hospital.
II. Data Collection
Data on the lifestyles and eating behaviors data of children were gathered from parents or guardians; these data included number of days of moderate physical activity per week and time spent watching TV per day (<1 hour, 1-2 hours, >2 hours). This information was used to identify respondents with sedentary lifestyles. Frequencies of overeating, eating precooked/frozen food, and eating out were ascertained with a food-frequency questionnaire. Questions about eating rate (fast, medium, or slow) and family meals (1/day, 4-6/week, 1-3/week, and 2-3/month) were constructed on the basis of previous studies. These factors were recategorized based on a frequency test.
Additional data on parental disease history, educational status, and current body mass index (BMI) were also obtained from the parents or guardians via questionnaire. If either parent had experienced a disease, it was included in the parental disease history.
III. Measurements
Medical examinations were conducted to collect information on anthropometric characteristics and to measure blood pressure and take blood samples. Height and waist circumference were measured to the nearest 0.1 cm, and weight was measured to the nearest 0.1 kg using a stadiometer and a calibrated scale with the child wearing only light clothing and no shoes. Blood pressure (BP) was measured on the right arm using a vital-signs monitor (Dinamap PRO 100; GE Healthcare, Little Chalfont, Buckinghamshire, UK) after the subject had been sitting comfortably for at least 5 minutes. Participants were instructed to fast for at least 8 hours prior to the examination in preparation for gathering data related to biochemical indices. Serum total cholesterol, high-density lipoprotein (HDL) cholesterol, triglycerides, and fasting glucose were measured with an automatic analyzer (model 7180; Hitachi, Tokyo, Japan).
BMI was calculated as weight divided by height squared (kg/m2). Subjects were categorized as obese (≥95th percentile), overweight (85-94th percentile), or normal (<85th percentile) according to their current BMI using sex- and age-specific criteria from the 2007 Korean Children and Adolescents Growth Standards [8].
We used the modified criteria developed by Cook et al. [9] to determine the clustering of risk factors for metabolic syndrome. Components of metabolic syndrome were judged to be present when at least one of the following risk factors was observed: waist circumference ≥90th percentile of subjects in this study adjusted for age and sex; systolic or diastolic BP ≥90th percentile of Korean children adjusted for age, sex, and height; fasting glucose ≥110 mg/dL, triglycerides ≥110mg/dL, and HDL cholesterol ≤40 mg/dL.
IV. Statistical Analysis
We compared the basic characteristics of normal, overweight, and obese participants using analysis of variance (ANOVA) and chi-square or Fisher's exact tests with trend analysis. The distribution of risk factors for metabolic syndrome was analyzed using a chi-square test. Bivariate and multivariate logistic regression analyses were conducted to evaluate the association between various factors and being overweight and obese. Factors with a significance of < 0.1 according to the bivariate logistic regression analysis were selected for a multivariate model. The multivariate logistic regression estimated the effect of lifestyle on being overweight and obese after adjusting for sex, age, education of the mother, maternal BMI, and parental diabetes. All analyses were conducted using SAS version 9.1 (SAS Inc., Cary, NC, USA). A p-value <0.05 was considered statistically significant.
RESULTS
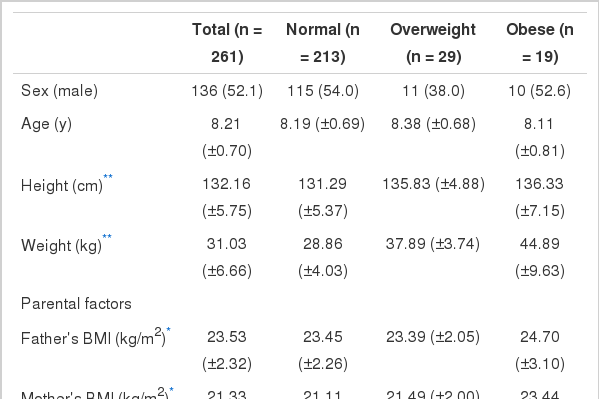
The 261 subjects were aged 8.21 ± 0.70 years (mean ± standard deviation [SD]) and included 136 boys (52.1%). The proportions of subjects who were overweight and obese were 11% (n = 29) and 7% (n = 19), respectively. Maternal BMI was significantly higher in obese children compared with that in mothers of normal-weight children (24.7 kg/m2 vs. 23.4 kg/m2). The obese group included a significantly higher proportion of children of parents with diabetes mellitus (p < 0.05) (Table 1).
High BP (90th percentile) was most the prevalent (28.0%) component of metabolic syndrome, whereas fasting glucose ≥110 mg/dL was the least common (0.8%). The overall prevalence of risk factors for metabolic syndrome was higher in the obese group than in the other groups. More than half of the overweight and almost all of the obese children had at least one risk factor for metabolic syndrome. Approximately 2% of all children and 21.1% of obese children had three or more risk factors, meeting the diagnostic criteria for metabolic syndrome (Table 2).
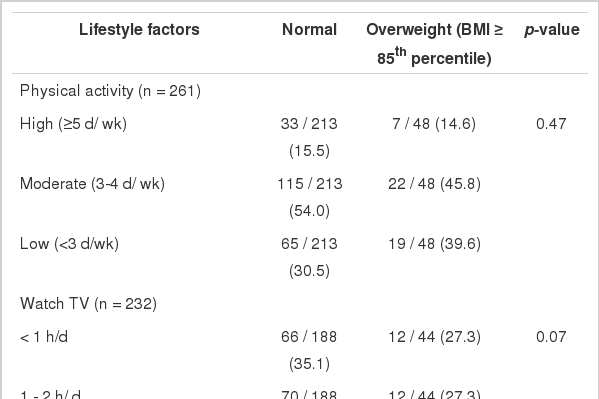
When we compared lifestyle factors among BMI categories, overweight and obese participants were combined into an overweight group because the number of obese subjects was small. Time spent watching TV tended to be higher in the overweight group than in the normal-weight group, and this difference reached marginal significance (p = 0.07). About half of the obese children spent ≥2 hours per day watching TV, whereas about 25% of the others spent that much time watching TV. The rate at which children ate differed significantly different between normal-weight and overweight groups. More children in the overweight than in the normal-weight group were reported by their parents to eat rapidly (41.7% vs. 15.1%). Children in the overweight group were also significantly more likely to overeat (60.9% vs. 27.5%) and significantly less likely to eat family meals (10.4% vs. 2.4%) compared with the normal group. However, the groups did not differ with respect to physical activity (Table 3).
Table 4 presents the associations between lifestyle-related factors and overweight or obesity. According to a bivariate analysis, those who spent >2 hours per day watching TV had an approximately two-fold greater risk of being overweight (odds ratio [OR], 2.19; 95% confidence interval [CI], 1.04 to 4.59). Those who ate fewer than three meals per month with their families had 4.18 (95% CI, 1.13 to 15.43) times the risk of being overweight than those who ate one meal with their families per day. Eating rate, overeating, and number of meals eaten with family remained significantly associated with being overweight in the multivariate logistic regressions analysis.
DISCUSSION
We found that eating behaviors such as eating rapidly, overeating, and participating in family meals only infrequently were significantly associated with preadolescents' risk for being overweight. Despite their young age, almost all obese children had at least one risk factor for metabolic syndrome, and one-quarter of obese children met the criteria for a diagnosis of metabolic syndrome.
The etiology of obesity is multidimensional. The dramatic increase in obesity during the past several decades suggests that environmental factors predominate over genetic effects [6]. Given that the incidence of obesity decreases with age, some studies have reported that becoming overweight at an early age has a more severe effect in adulthood than later overweight status has [10]. In the present study, children who were overweight or obese were at a greater risk for developing the risk factors for metabolic syndrome, a finding that was consistent with the results of previous studies [9]. Thus, this result provides additional evidence for the relationship between obesity and metabolic dysfunction. It also shows that additional studies are needed to identify the risk factors that can be modified to prevent childhood obesity. Potentially modifiable risk factors for obesity involve physical activity, watching TV, and an unhealthy diet. However, several interventional studies on increased physical activity and diet control have not provided consistent results or succeeded in modifying adult behavior. Because lifestyles and behaviors are established early in life, strategies to eliminate and/or modify the risk factors for obesity should be implemented during preadolescence [11].
Obesity results from an imbalance between energy intake and energy expenditure. Epidemiological studies have shown that physical inactivity and a sedentary lifestyle are independently related to the development of obesity in children [12], adolescents [13], and adults [14]. Decreased opportunities for physical activity may contribute to obesity. Indeed, watching TV results in a lower metabolic rate than do other sedentary activities such as reading, writing, and playing board games [15]. One study showed that watching TV for long periods was associated with lower levels of HDL cholesterol and higher levels of leptin [3]. According to the Nurses' Health Study, watching TV for >2 hours per day was associated with a 23% increase in obesity in adult women [14]. One cohort study reported that >8 hours of TV watching per week at 3 years of age increased the risk for obesity at age 7 by 1.6 times [4]. In the present study, those who spent >2 hours per day watching TV had twice the risk of being overweight (95% CI, 1.04 to 4.59), but this effect disappeared after adjusting for other factors. Furthermore, unlike previous studies [5], we could not identify the risk posed by physical inactivity for being overweight. One longitudinal study showed that physical inactivity appeared to be the result of obesity rather than its cause. The authors stated that promoting physical activity has been largely unsuccessful [16]. Research on the etiology of obesity has been hampered by an inability to accurately assess such characteristics of physical activity as intensity, patterns, and quantity. Thus, the relationship between inactivity and obesity may reflect other, unknown factors and not indicate direct causality. Recently, an article reviewing studies that attempted to modify physical activity reported that physical interventions to deal with childhood obesity are unlikely to have a significant effect in improving BMI, although such interventions do have other beneficial health effects [17].
Constant commercial advertisements accompanied by prolonged TV watching may lead to unhealthy eating patterns such as snacking, which typically involves a higher caloric intake than do more healthy eating habits [18-20]. This change to an unhealthy diet including low fiber intake, a lack of fruits and vegetables, increased sugar, and more convenience food is also widely believed to have contributed to the child obesity epidemic [21]. Moreover, eating behaviors and energy intake are also related to the development of obesity. Although one review article stated that unhealthy eating habits such as eating outside of the home, participating in few family meals, eating rapidly, and overeating may affect total caloric intake [6], only a few studies on eating behaviors and child obesity have been conducted. Consistent with previous findings, the present study revealed an association between being overweight and eating rapidly [11,22]. One study showed that those who have eaten rapidly from a young age also weighed more, had higher BMIs, and consumed more energy [23]. Several randomized controlled trial studies have also found that eating more slowly and reducing total food intake were useful for obese adolescents [24]. Because an abnormally rapid rate of eating may lead to additional eating before the stomach senses fullness, the rate of eating and the quantity of energy consumed may be positively related [23]. In the present study, eating rate appears to have been associated with overeating, as almost 60% of children who ate rapidly also engaged in overeating (data not shown).
Unfavorable family circumstances have also been associated with overweight among children [25]. The frequency with which families eat together has decreased as the consumption of fast food and unhealthy meals have increased [6]. Mealtimes spent with parents contribute to the nutritional beliefs and attitudes held by children [26]. Several studies have reported that children who attended fewer family meals were more likely to be overweight [27,28]. Parents influence what, when, and how much children eat and can also directly guide their children's eating behaviors [26]. However, further research is needed to clarify the mechanisms by which family meals affect children's long-term health.
This study had several limitations. First, we used self-reports to gather data on factors related to lifestyle, which may have influenced the validity of the results. However, previous studies have found that self-report data are fairly accurate [29]. Further studies are needed to verify the validity of using a self-reporting method to gather information on lifestyles. Second, we did not investigate energy intake. Third, the results were gathered from a cross-sectional sample of elementary school students, thus rendering it difficult to generalize our results. Finally, the small sample resulted in low statistical power.
Nevertheless, our study had several advantages over previous similar studies because it considered various specific eating behaviors and focused on preadolescents, who have been relatively neglected by previous research. Childhood obesity rates may differ in Asian and Western countries because of the Westernized diet and environment. Thus, this study has value because few studies have been conducted on the distribution of the risk factors for metabolic syndrome and the prevalence of childhood obesity in the Asia-Pacific region. Finally, this study considered factors that are preventable and subject to efforts at prevention.
This study showed that children who were overweight or obese were considerably more likely to engage in unhealthy eating behaviors. Our results have two clear implications. First, the acquisition of healthy eating habits early in life can contribute to weight control and the reduction of obesity. Second, participation in family meals may be important for preventing childhood obesity.
ACKNOWLEDGEMENTS
This work was supported by a National Research Foundation of Korea Grant funded by the Korean Government (2009-0064004) and the Ministry of Health & Welfare (02-PJ1-PG1-CH03-0001).
Notes
The authors have no conflicts of interest with the material presented in this paper.
This article is available at http://jpmph.org/.