Articles
- Page Path
- HOME > J Prev Med Public Health > Volume 48(1); 2015 > Article
-
Original Article
Factors That Affect Suicidal Attempt Risk Among Korean Elderly Adults: A Path Analysis - Junsoo Ro1, Jongheon Park2, Jinsuk Lee1,3, Hyemin Jung1
-
Journal of Preventive Medicine and Public Health 2015;48(1):28-37.
DOI: https://doi.org/10.3961/jpmph.14.030
Published online: January 14, 2015
1Department of Health Policy and Management, Seoul National University College of Medicine, Seoul, Korea
2National Health Insurance Service, Seoul, Korea
3Institute of Health Policy and Management, Medical Research Center, Seoul National University, Seoul, Korea
- Corresponding author: Jongheon Park, MD, PhD 311 Dongmak-ro, Mapo-gu, Seoul 121-749, Korea Tel: +82-2-3270-9696, Fax: +82-2-3275-8022 E-mail: jmhoney@chol.com
• Received: July 3, 2014 • Accepted: December 3, 2014
Copyright © 2015 The Korean Society for Preventive Medicine
This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/bync/3.0/) which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
ABSTRACT
-
Objectives:
- Among the Korean elderly (those 65 years of age and older), the suicide rate is 80.3/100 000 people, which is ten times higher than the Organization for Economic Cooperation and Development average. Because South Korea is rapidly becoming an aging population, this high elderly suicidal rate will only get worse. Although the size of the elderly suicide problem is quite large, previous research in South Korea has surveyed restricted areas and not the entire country. Even though the factors that affect elderly suicide are complicated, there has been little research into these influencing factors. Thus, this research uses the national survey data (Community Health Survey) that was obtained in 2009. Additionally, we analyze factors affecting elderly suicidal ideation and attempts as well as the paths of these effects.
-
Methods:
- Community Health Survey data obtained by the Korea Centers for Disease Control and Prevention in 2009 was used for this study. We additionally examined the factors that affect suicide with chi-squared tests, t-tests, Pearson’s correlation test, and path analysis.
-
Results:
- Depressive symptoms and suicidal ideation are the only factors that directly affect suicidal attempts. Demographic, behavioral, and physical activity factors have indirect effects on suicidal attempts.
-
Conclusions:
- Depression has the strongest influence on suicidal ideation and attempts. Demographic, behavioral, and physical activity factors affect suicidal attempts mostly through depressive symptoms. In addition, there is a path that suggests that demographic, behavioral, and physical activity factors affect suicidal attempts not through depression symptoms but only through suicidal ideation. This means that the elderly who do not have depression symptoms attempt suicide according to their own situations and characteristics.
- Each year, one million people die from suicide worldwide [1]. Suicide is one of the biggest causes of death among the economically active population (15 to 44 years old), and it is the second highest cause of death among the population aged 15 to 19 years old [2]. Globally, the health burden of suicide is projected to gradually increase from 1.8% in 1998 to 2.4% in 2020 [3]. In 2010, the Korean suicide rate was 33.5 persons per 100 000 people, and this is the highest rate among Organization for Economic Cooperation and Development (OECD) countries. Furthermore, it is 2.6 times more than the OECD average. The Korean suicide rate steadily increased from 1995 to 2009. According to OECD health data, the suicide rate of OECD countries has decreased since 2009, but the suicide rate has increased in only 7 countries, including South Korea, Chile, Japan, and Mexico [4]. The suicide rate among the elderly population over the age of 65 was the highest, at 80.3 persons per 100 000 people in 2009 among all OECD countries. This was about 10 times higher than that of the OECD average. During the same period of time, the elderly suicide rate in other OECD countries showed no significant change and remained constant. By contrast, Switzerland showed a small increase at 1.1 times greater, and this was the second biggest increment after South Korea. Similarly, the suicide rate among the elderly population has steadily increased at a rate much greater than that for economically active children and youth.
- Unlike the suicide of youth, which is generally caused by a single factor (lack of academic achievement, breakups, or disagreements with parents or teachers), suicide among the elderly has multifactorial causes, rather than a single reason [5,6]. The elderly are vulnerable to suicide as they are exposed to a number of factors that influence suicide, such as loneliness after losing spouses or relatives, chronic diseases, and financial hardship [7]. Previous studies conducted abroad have suggested depression is the factor that has the greatest impact on suicide among the elderly population. Additionally, depression in the elderly is typically due to social isolation, bereavement, restrict of daily living, physical decline, and various other chronic disease-related reasons [8].
- The previous studies by Choi and Kim in 2008 [9], and the study by Bae and Um in 2009 [10] studied factors that affect suicide among the elderly and identified factors that influence Korean elderly suicide; however, as the study data included the elderly population of only some areas, it was hard to generalize the results.
- Although the study by Yoon et al. in 2010 [11] identified stress’s path to suicide through analysis, it was limited in its understanding of the specific characteristics of the elderly, as it is surveyed in limited area. In a 2008 study by Kim and Hwang [12], senile disease and depression were sub-divided, and a structural model was used to analyze their effects on suicidal ideation. However, the study was limited in making generalizations, as only the elderly from Seoul were studied. Since only senile disease and depression were used as variables, another limitation of this study is that other socioeconomic factors related to suicide were not analyzed.
- In a 2007 study by Kim and Kim [13], a detailed analysis was performed on the relationship between suicidal ideation and factors that can influence suicide, such as state of health, state of finance, stress, and self-esteem from which the paths of the factors that affect suicidal ideation among the elderly were identified. However, since regression coefficients were used instead of structural equations, there were limitations in the inability to obtain the model’s fitness. Furthermore, all three aforementioned studies investigated only suicidal ideation for their studies and were limited in not investigating suicidal attempts. Studies on suicides among the elderly have been conducted in South Korea to examine the influencing factors and their paths, but there are some limitations in representativeness and causality.
- The present study aimed to provide evidence and basic data for suicide prevention policies for the elderly by conducting a structural equation analysis using the 2009 Korean Community Health Survey (KCHS) to identify the relationships and paths between the factors that affect elderly suicidal ideation and attempts. Therefore, the subject of the present study comprises identifying factors that affect suicidal ideation and attempts among Korean elderly aged 65 years or older and analyzing the interactions between the factors and the paths that lead to suicidal attempts.
INTRODUCTION
- Study Population
- The present study used the national data from the 2009 KCHS, which was conducted in 253 community health centers between September and November 2009. The 2009 KCHS surveyed adults aged 19 years or older, with each community health center surveying an average of 900 participants. The households selected as samples were visited by a trained surveyor for one-on-one interviews, and the survey was conducted using a paper questionnaire. The total number of participants who completed the final questionnaire was 230 715. The elderly population of those 65 years or older, who were the subjects for this study, totaled 51 685, among which 49 357 were included in the analysis after those who had missing survey answers were excluded [14].
- Definition of Variables
- The dependent variable, suicidal attempt, was defined as cases in which the response indicated suicide was actually attempted within the past year.
- Suicidal ideation was defined as cases in which the response indicated they had had thoughts of wanting to die within the past year. Depression symptoms were measured using the Center for Epidemiologic Studies Depression Scale (CES-D). The CES-D was developed by Radloff, and it consists of 20 self-reporting questions. It is designed for use in measuring depression symptoms within a general community population [15]. The maximum score is 60 points, and higher scores indicate higher degrees of depression. In the present study, the CES-D scores were used asis for the analysis.
- Household income was defined as all income, including wages, property income, pension, interest income, government subsidies, and allowances from relatives or children, divided by the number of household members. Determination of a oneperson household was based on the response to the household type question in the survey, with those who responded ‘oneperson household’ being defined as ‘elderly living alone’ and all others defined as ‘elderly not living alone.’ Although the KCHS divides households into several different types, the households were defined as above since a previous study indicated the factor affecting suicide among the elderly was influenced by the presence or absence of a spouse or a co-habitant. In terms of job status, those who responded ‘homemaker’ or ‘unemployed’ on the occupation question were defined as ‘not having a job,’ and all others were defined as ‘have a job.’ In the KCHS, jobs were classified according to standard job types, but since previous studies proposed that effects of jobs on suicide among the elderly were determined by having a job or not having one rather than by job type, we used the dichotomous variable of having a job/not having a job [16-18].
- In the 2009 KCHS, alcoholic drinking behavior was surveyed using the Alcohol Use Disorder Identification Test, which is an instrument developed by the World Health Organization that measures alcohol dependency and problem drinking. Alcohol Use Disorder Identification Test assessment results were classified as 0 to 7 points being the ‘normal’ group; 8 to 12 points indicating ‘hazardous drinking’; 13 to 19 points indicating ‘harmful drinking’ group; and 20 to 40 points indicating ‘suspicious alcohol dependency.’ Anyone who had smoked 5 packs (100 cigarettes) or more in their lifetime and currently smoked was classified as a ‘current smoker,’ while everyone else belonged to the ‘current non-smoker’ group.
- In terms of physical activity, a ‘moderate or greater physical activity performer’ was defined as someone who had performed physical activity consisting of a single session of 20 minutes or more 3 or more days in the past week or a single session of 30 minutes or more performed 5 or more days per week. A ‘walking performer’ was one who participated in walking sessions of 30 minutes or more 5 or more days per week. Those who engaged in any of the physical activities mentioned above were defined as being in the ‘physical activity performer’ group, and those who did not were included in the ‘no physical activity performer’ group.
- Concerning doctor diagnosis of severe diseases, anyone who had responded that they had been diagnosed by a doctor with stroke, myocardial infarction, or angina pectoris were defined as having a ‘doctor’s diagnosis of severe disease experience,’ and those who responded that they had not were defined as being part of the ‘severe disease non-experienced’ group. Concerning doctor diagnosis of mild diseases, those who had been diagnosed by a doctor with either hypertension or diabetes were defined as being part of the ‘doctor diagnosis of mild disease experience’ group, and those who had never been diagnosed with either of these disease were separated into the ‘mild disease non-experience’ group. Self-rated health status was analyzed using a 5-point scale, with responses of ‘very good,’ ‘good,’ ‘normal,’ ‘poor,’ and ‘very poor’ [14,19].
- Research Models
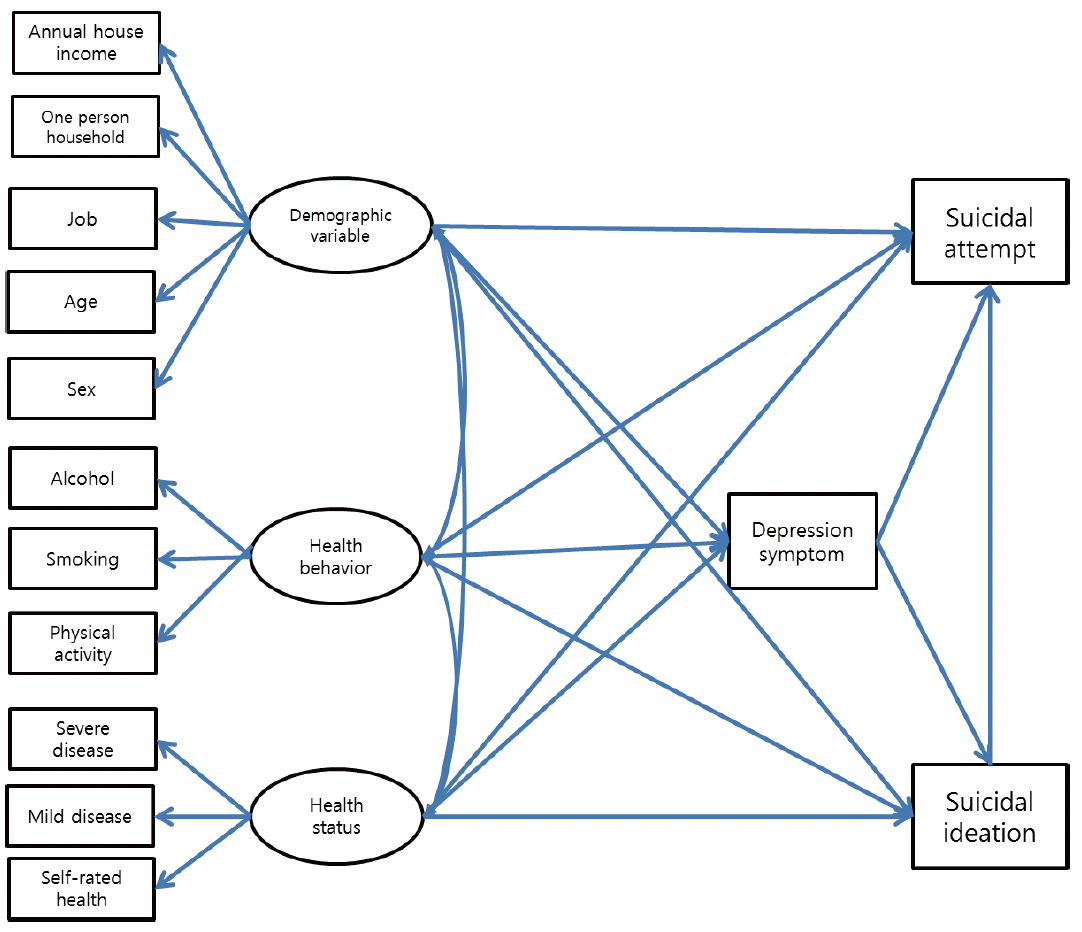
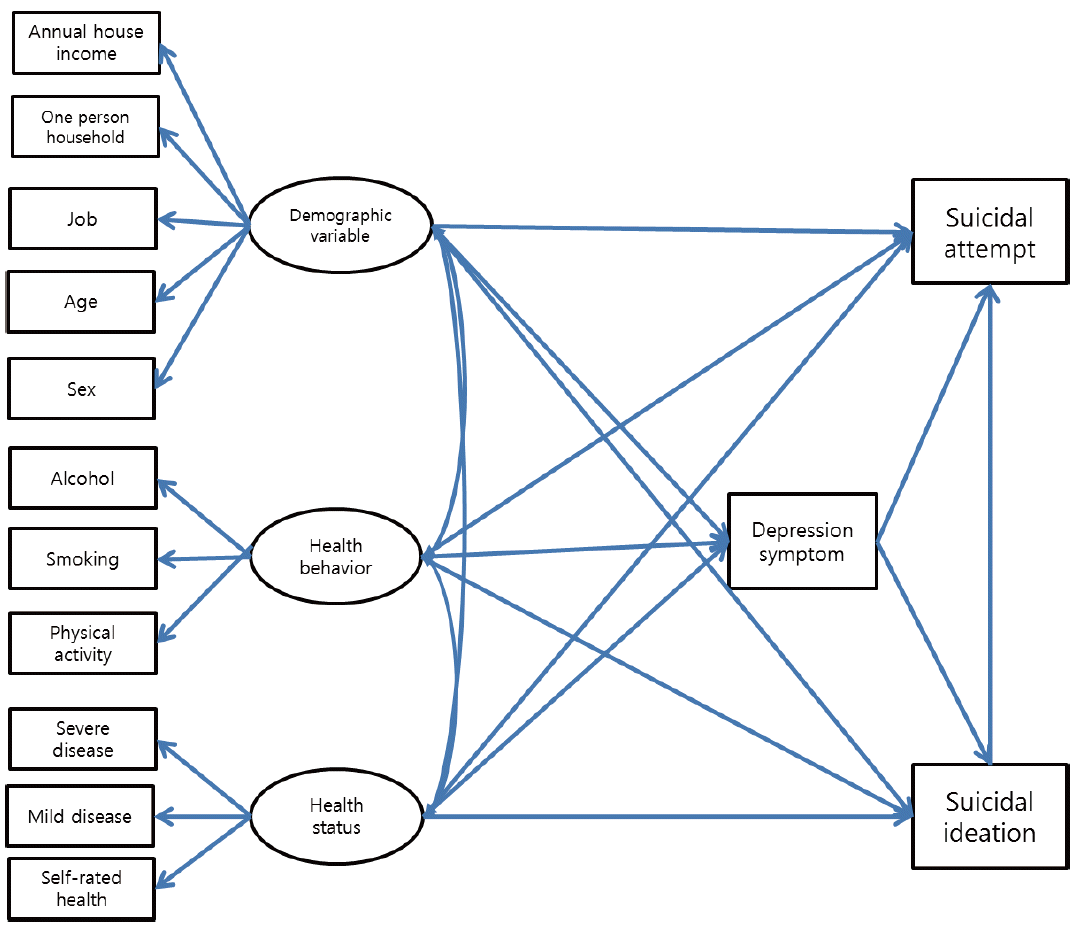
- Using previous studies as the basis, the research and competition models were constructed as follows. A structural model that directly affected suicidal ideation and attempts from demographic, health behaviors, and physical health status factors, as well as indirect effects on suicidal ideation and attempts by mediation through depression symptoms was established as the research model. A structural model with direct effects of demographic, health behavior, and physical health status on suicidal ideations, but only indirect effects on suicidal attempts by mediation through depression symptoms was established as the competition model (Figures 1 and 2). The fitness of the constructed structural models was assessed using fit indices. Many different fit indices may be used to assess the research model’s fitness. Among those, the present study used the absolute fitness indices x2 and the Root Mean Squared Error of Approximation (RMSEA), along with the Goodness-of-fit Index (GFI), which are commonly used indices. The criteria was GFI>0.9 and RMSEA <0.05 for good model fitness, <0.08 for marginal fitness, and <0.1 for normal fitness [20]. Lower Parsimonious Goodness-of-fit Index (PGFI), indicated better model fitness.
- Analysis Method
- The variables that can affect suicidal attempts among the elderly were selected through reviews of previous studies, and univariate analysis was performed using x2-test to examine the frequency of each variable and their relationships with suicidal attempts, while the degree of relevance and directionality of each variable and suicidal attempts were examined via correlation analysis. Afterwards, path analysis was performed on both the research and competition models. SPSS version 20.0 (IBM Corp., Armonk, NY, USA) was used for the frequency analysis, x2-test, and correlation analysis, while AMOS version 20.0 (IBM Corp., Armonk, NY, USA) was used for path analysis.
METHODS
- Statistics on Suicidal Attempt and Relevant Variables
- When the relevance of the general characteristics of the elderly in this study and suicidal attempt were analyzed via x2-test, the results indicated that lower household income, one-person household, no job, current smoker, physical activity non-performer, doctor’s diagnosis of severe disease experience, low self-rated health status, high depression symptom score, and suicidal ideation were significantly associated with suicidal attempts (Table 1).
- The results of the examination of the degree of relevance and directionality between the study variables, the mean, standard deviation, and correlations among the entire group are shown in Table 2. The variable that had the highest correlation with suicidal attempt was suicidal ideation (0.147, p<0.01), followed by depression symptoms (0.127, p<0.01). The variable that showed the highest correlation with suicidal ideation was depression symptoms (0.410, p<0.01), followed by self-rated health status (0.241, p<0.01). The highest depression symptom correlations were seen with suicidal ideation (0.410, p<0.01) and self-rated health status (0.270, p<0.01). The correlations between suicidal attempt, suicidal ideation, and depression symptoms were high (Table 2).
- Assessment of the Research Model’s Fitness
- In order to test the model that explains the structural relationship between suicidal attempts and the relevant variables, comparative analysis on the fitness of research and competition models was conducted to look for the optimal model.
- To compare the research model to the competition model, the fit indices of both models were compared (Table 2). The p-value of x2 was <0.001 in both models, showing they were not fit, but because x2 is affected by sample size and complexity, there is a limitation in obtaining an appropriate x2 value when the sample size is big or the model is complex. The GFI values for both models were 0.938, indicating marginal model fitness. The RMSEA value, which is least affected by sample size, was 0.083 and 0.081 for research and competition models, respectively, which showed marginal fitness for both models. PGFI which is useful for comparing two models, was 0.581 and 0.608 for the research and competition models, respectively. This indicated that the research model was lower. Both models were shown to be fit by the absolute fitness index, with little difference between their values; hence, we selected the model that was better according to the parsimony fitness index (Table 3).
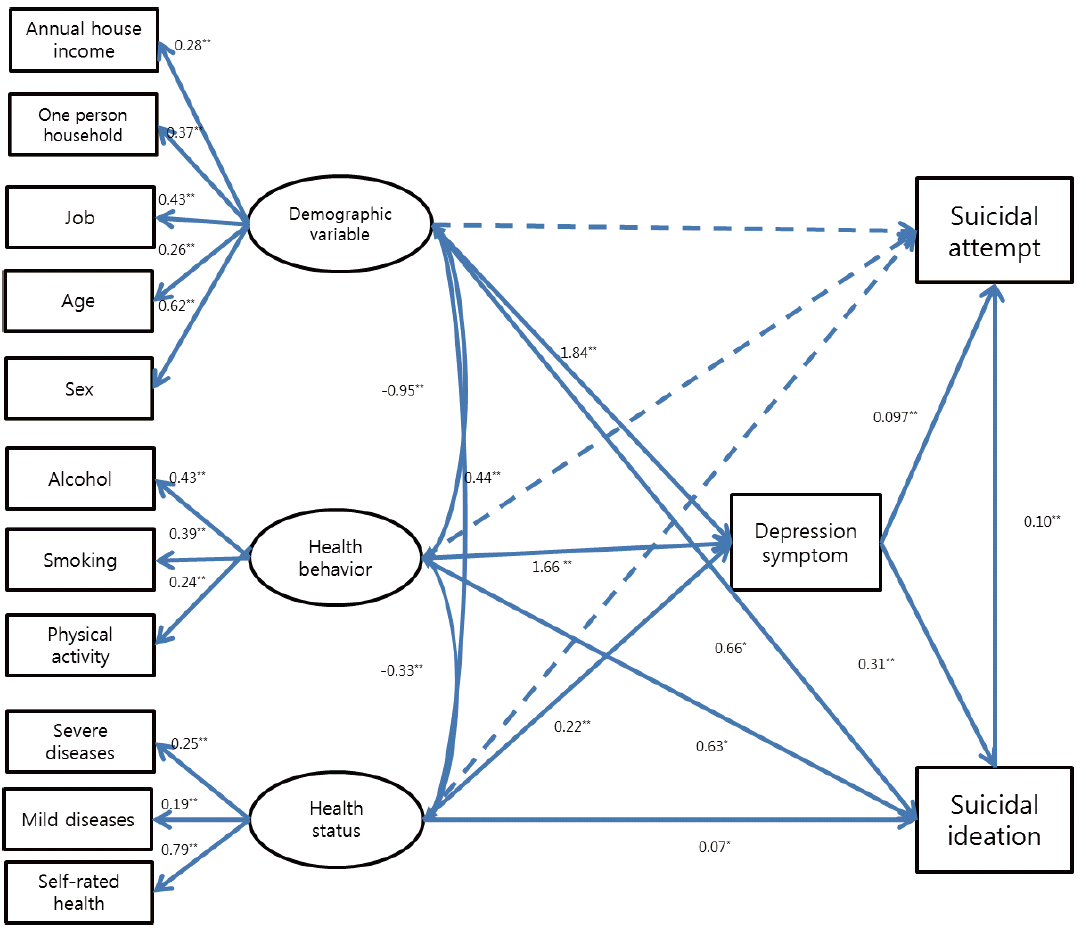
- Path analysis was performed with the research model that was selected as the final model. The results and standard coefficient values are shown in Figure 3.
- Concept validity, which confirms whether the observed variables that result from confirmatory factor analysis and constitute the latent variables are made with the proper concept and definition, was also confirmed. Although the standardized values of the observed variables that constitute each latent variable were significant, only partial concept validity was obtained, as no standardized coefficients of observed variables exceeded 0.5.
- Path Coefficients That Affect Suicidal Attempts
- Among the direct effects on suicidal attempts, only suicidal ideation and depression symptoms were statistically significant. suicidal ideation was β=0.100 (p<0.001), and the value for depression symptoms was β=0.097 (p<0.001). The trend toward suicidal ideation affecting attempted suicide was slightly higher, but this difference was not significant. Behavioral, demographic, and physical health status factors did not show statistically significant direct effects on attempted suicide.
- The indirect effects on suicidal attempts, demographic (β= 0.301), physical health status (β=0.035), and health behavior (β=0.275) factors were statistically significant. In order to identify which variable each factor uses for mediation in the exertion of indirect effects, direct effects were separated out. In the case of demographic variables, indirect effects were statistically significant in all cases of mediation through depression symptoms (β=0.178, p<0.001), depression symptoms and suicidal ideation (β=0.0569, p<0.001) and only suicidal ideation (β=0.0663, p< 0.001). Among health behavior variables, indirect effects were statistically significant in all cases of mediation through depression symptoms (β=0.1608, p<0.001), depression symptoms and suicidal ideation (β=0.0513, p<0.001) and only suicidal ideation (β=0.0629, p<0.001). Among physical health status variables, indirect effects were statistically significant in all cases of mediation through depression symptoms (β=0.021, p<0.001), depression symptoms and suicidal ideation (β=0.0067, p<0.001) and only suicidal ideation (β=0.0073, p<0.001). Depression symptoms were statistically significant when mediation occurred through suicidal ideation (β=0.031, p<0.001).
- In terms of total effect on suicidal attempts, health behavior factors had the biggest effect (β=0.339), followed by demographic factors (β=0.331). Physical health status factors had the smallest effect (β=0.027) (Table 4).
RESULTS
- The present study aimed to identify the factors that affect suicide among the elderly, aged 65 years or older and the paths that lead to suicidal attempts.
- In the correlation analysis that was performed to examine the relationships between the different influencing variables, relevance appeared to be the highest in the relationships between suicidal attempt, suicidal ideation, and depression symptoms. In the path analysis, suicidal ideation (β=0.100) was shown to have the biggest direct effect on suicidal attempts. These results are consistent with the results from a previous study that indicated suicidal ideation, suicidal attempts, and acts of suicide are concepts that form a series leading from one to the next [2]. The second biggest direct effect, after suicidal ideation, was seen in depressive symptoms (β=0.097). Depression symptoms can affect suicidal attempts through directly, but they can also affect them indirectly by mediation through suicidal ideation. In addition, demographic factors, along with health behavior and physical health status variables affect suicidal ideation and attempts by mediation through depression symptoms. These results are consistent with previous studies that identified depression as the single biggest cause of suicidal attempts and ideation [8,21-24].
- Although demographic factors do not directly affect suicidal attempts (p>0.05), they were shown to indirectly affect it by mediation through depression symptoms and suicidal ideation (β=0.301). Among the demographic factors, being female, 75 years or older, having a low household income, living in a oneperson household, and having no job having had a great effect on depression and suicidal ideation. This was in agreement with previous studies [9,25]. Most of the demographic factor effects acted indirectly through depression symptoms.
- Health behavior factors do not have direct effects on suicidal attempts either (p>0.05), but they were shown to indirectly affect suicidal attempt by mediation through depression symptoms and suicidal ideations (β=0.275). This is in agreement with a previous study that the elderly who are heavy smokers show a higher rate of suicidal attempts and lower levels of physical activity. A previous study about health behavior and suicide in the elderly, also identified that heavier drinking among the elderly led to higher suicidal ideation and that elderly who have suicidal ideation exhibited higher frequencies and amounts of drinking than those who did not have suicidal ideation [26].
- Similarly, physical health status factors do not affect suicidal attempts directly (p>0.05), but they show indirect effects by mediation through depression symptoms and suicidal ideation (β= 0.035). This is consistent with results from a previous study that stated poor health affects depression and suicidal ideation [8].
- The present study analyzed the effects of demographic factors, health behavior factors, and physical health status factors on depression symptoms, suicidal ideation, and suicidal attempts. Only a few existing studies have looked at suicidal ideation and suicidal attempts simultaneously. Many studies used suicidal ideation as an outcome factor by defining suicidal ideation and attempts as a series of events, in which suicidal attempts were predicted when suicidal ideation was present. However, the present study used suicidal ideation and attempts simultaneously to determine whether each factor directly affected suicidal attempts or indirectly affected suicidal attempts through suicidal ideation. From the study results, it was determined that the factors that directly affected on suicidal attempts among the elderly were depression symptoms and suicidal ideation, with demographic factors, health behaviors, and physical health status factors having indirect effects on suicidal attempts by mediation through depression symptoms and suicidal ideation.
- The present study showed that depression symptoms affected suicidal ideation and attempts directly and indirectly, whereas the effects on suicidal attempts from demographic factors and health behaviors and physical health status factors were mostly mediated through depression symptoms. This finding reconfirmed depression as the single most influential variable for suicidal attempts among the elderly, and this finding is similar to what was found in other studies [8,20-22].
- Moreover, although demographic factors and health behaviors and physical health status factors showed indirect effects being mediated through depression symptoms, which made up most of the effects seen in each variable, each variable also indirectly affected suicidal ideation by mediation through suicidal ideation and not by passing through depression symptoms. This shows an improvement from the previous studies, which emphasized the importance of depression in elderly suicides and points to the fact that suicidal attempts among the elderly can occur without experiencing depression as a result of suicidal ideation that develops from the individual characteristics of, or the situations faced by, the elderly.
- The present study used national data with representativeness. Previous studies examining suicide among the elderly were limited to surveying the elderly only in specific regions, due to study restrictions of the study, and they had difficulties securing representativeness because of this. By using the national data from the 2009 KCHS, the present study was able to secure representativeness. Furthermore, by using structural equations, we were able to obtain fitness of the overall model that other studies were not able to obtain, and this made it possible to overcome the disadvantages of constructing a path model with only significant regression coefficients extracted during path analysis via regression analysis.
- The present study’s limitations are as follows. First, since suicide planning was not investigated, it was not included in the study. Typically, suicide follows the sequence of suicidal ideation and suicide planning before going on to suicidal attempt. However, because KCHS did not investigate suicide planning, it was not included in the structural equation. Future studies should examine suicidal ideation, suicide planning, and suicidal attempts all at once to show their connections to the individual variables.
- Second, the study was conducted cross-sectionally. Therefore, the causal relationships between the variables could not be clearly stated. In order to clarify the causal relationships between the variables, longitudinal studies, such as cohort studies, are needed.
- Third, a path analysis was performed using the primary results from this study. However, since the mixed-samples KCHS data were used, mixed-sample analysis should have been performed; however, the path analysis using AMOS did not offer any methods for analyzing mixed samples.
- In conclusion, depression symptom is the biggest single factor on elderly suicidal attempt. But, there is a path that led to suicidal attempt by mediation through suicidal ideation without depression symptom. It means that individual characteristics or situation can lead to suicidal attempts without depression.
DISCUSSION
-
Conflict of Interest
The authors have no conflicts of interest with the material presented in this paper.
Notes
Table 1.General characteristics
| Variables | Category | Frequency | % |
Suicide attempt |
p-value1 | |
|---|---|---|---|---|---|---|
| Case | % | |||||
| Sex | Male | 20 053 | 40.6 | 120 | 0.6 | 0.49 |
| Female | 29 304 | 59.4 | 191 | 0.65 | ||
| Age (y) | 65-74 | 32 480 | 65.8 | 208 | 0.64 | 0.72 |
| ≥75 | 16 877 | 34.2 | 103 | 0.61 | ||
| Annual house income | 1st quartile (poor) | 11 743 | 23.8 | 118 | 1 | <0.001 |
| 2nd quartile | 12 301 | 24.9 | 70 | 0.57 | ||
| 3rd quartile | 12 925 | 26.2 | 69 | 0.53 | ||
| 4th quartile (rich) | 12 388 | 25.1 | 54 | 0.44 | ||
| One person household | Yes | 10 254 | 20.8 | 89 | 0.87 | 0.001 |
| No | 39 103 | 79.2 | 222 | 0.57 | ||
| Job | Yes | 16 973 | 34.4 | 77 | 0.45 | <0.001 |
| No | 32 384 | 65.6 | 234 | 0.72 | ||
| Alcohol | Normal (0-7) | 44 559 | 90.3 | 272 | 0.61 | 0.11 |
| Hazardous drinking (8-12) | 3382 | 6.9 | 26 | 0.77 | ||
| Harmful drinking (13-19) | 699 | 1.4 | 4 | 0.57 | ||
| Suspicious alcohol dependency (20-40) | 717 | 1.5 | 9 | 1.26 | ||
| Smoking | Smoker | 7317 | 14.8 | 66 | 0.9 | 0.002 |
| Non-smoker | 42 040 | 85.2 | 245 | 0.58 | ||
| Physical activity | Perform | 27 704 | 56.1 | 146 | 0.53 | 0.001 |
| Not perform | 21 653 | 43.9 | 165 | 0.76 | ||
| Severe disease | Experienced | 5598 | 11.9 | 63 | 1.13 | <0.001 |
| Not experienced | 43 459 | 88.1 | 248 | 0.57 | ||
| Mild disease | Experienced | 25 357 | 51.4 | 157 | 0.62 | 0.78 |
| Not experienced | 24 000 | 48.6 | 154 | 0.64 | ||
| Self-rated health status | Very bad | 6031 | 12.2 | 99 | 1.64 | <0.001 |
| Bad | 18 878 | 38.2 | 144 | 0.76 | ||
| Normal | 15 488 | 31.4 | 42 | 0.27 | ||
| Good | 8371 | 17 | 25 | 0.3 | ||
| Very good | 589 | 1.2 | 1 | 0.17 | ||
| CES-D score | ≥21 (depression symptom) | 5599 | 11.3 | 119 | 2.13 | <0.001 |
| <21 (normal) | 43 758 | 88.7 | 192 | 0.44 | ||
| Suicidal ideation | Experienced | 7924 | 16.1 | 260 | 3.28 | <0.001 |
| Not experienced | 41 433 | 83.9 | 51 | 0.12 | ||
Table 2.Correlation matrix within the variables1
| Sex | Age | Annual house income | One person household | Job | Alcohol | Smoking | Physical activity | Severe disease | Mild disease | Self-rated health status | Depression symptom | Suicidal ideation | Suicidal attempt | |
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Sex | 1 | |||||||||||||
| Age | 0.072** | 1 | ||||||||||||
| Annual house income | 0.094** | 0.101** | 1 | |||||||||||
| One person household | 0.244** | 0.106** | 0.470** | 1 | ||||||||||
| Job | 0.267** | 0.240** | 0.035** | 0.090** | 1 | |||||||||
| Alcohol | -0.317** | -0.087** | -0.030** | -0.075** | -0.149** | 1 | ||||||||
| Smoking | -0.339** | -0.037** | 0.004 | -0.043** | -0.101** | 0.222** | 1 | |||||||
| Physical activity | -0.119** | -0.158** | -0.050** | -0.050** | -0.200** | 0.060** | 0.026** | 1 | ||||||
| Severe disease | -0.032** | 0.020** | 0.004 | -0.017** | 0.095** | -0.020** | -0.020** | -0.063** | 1 | |||||
| Mild disease | 0.088** | 0.018** | 0.004 | 0.041** | 0.120** | -0.032** | -0.089** | -0.041** | 0.131** | 1 | ||||
| Self-rated health status | 0.165** | 0.135** | 0.186** | 0.094** | 0.201** | -0.079** | -0.048** | -0.207** | 0.192** | 0.147** | 1 | |||
| Depression symptom | 0.105** | 0.070** | 0.135** | 0.106** | 0.134** | -0.022** | -0.007 | -0.130** | 0.105** | 0.039** | 0.270** | 1 | ||
| Suicidal ideation | 0.100** | 0.063** | 0.116** | 0.093** | 0.101** | -0.014** | 0 | -0.102** | 0.082** | 0.044** | 0.241** | 0.410** | 1 | |
| Suicidal attempt | 0.003 | -0.002 | 0.024** | 0.015** | 0.016** | 0.009* | 0.014** | -0.015** | 0.020** | -0.001 | 0.049** | 0.127** | 0.147** | 1 |
| Mean | 0.59 | 0.34 | 1.47 | 0.21 | 0.66 | 0.14 | 0.15 | 0.56 | 0.12 | 0.51 | 2.43 | 0.11 | 0.16 | 0.01 |
| Standard deviation | 0.491 | 0.474 | 1.108 | 0.406 | 0.475 | 0.486 | 0.355 | 0.496 | 0.324 | 0.5 | 0.949 | 0.317 | 0.367 | 0.079 |
Table 3.Fit index between research and competition model1
| df | x2 test (p-value) | GFI | RMSEA | PGFI | |
|---|---|---|---|---|---|
| Research model | 65 | < 0.001 | 0.938 | 0.083 | 0.581 |
| Competition model | 68 | < 0.001 | 0.938 | 0.081 | 0.608 |
Table 4.Direct, indirect, and total effect in research variables and paths1
| Paths | Direct effect | Indirect effect | Total effect | |||
|---|---|---|---|---|---|---|
| Demographic variable | →Suicidal attempt | 0,03 | 0,301* | 0,331 | ||
| Demographic variable | →Depression symptom | →Suicidal attempt | 0,178** | |||
| Demographic variable | →Depression symptom | ->Suicidal ideation | →Suicidal attempt | 0,0569* | ||
| Demographic variable | ->Suicidal ideation | →Suicidal attempt | 0,0663* | |||
| Health behavior | →Suicidal attempt | 0,064 | 0,275 * | 0,339 | ||
| Health behavior | →Depression symptom | →Suicidal attempt | 0,1608** | |||
| Health behavior | →Depression symptom | ->Suicidal ideation | →Suicidal attempt | 0,0513* | ||
| Health behavior | ->Suicidal ideation | →Suicidal attempt | 0,0629* | |||
| Physical health status | →Suicidal attempt | -0,008 | 0,035** | 0,027 | ||
| Physical health status | →Depression symptom | →Suicidal attempt | 0,021** | |||
| Physical health status | →Depression symptom | ->Suicidal ideation | →Suicidal attempt | 0,0067** | ||
| Physical health status | ->Suicidal ideation | →Suicidal attempt | 0,0073** | |||
| Depression symptom | →Suicidal attempt | 0,097** | 0,045** | 0,128** | ||
| Depression symptom | ->Suicidal ideation | →Suicidal attempt | 0,045** | |||
| Suicidal ideation | →Suicidal attempt | 0,100** | 0,100** |
- 1. World Health Organization. Public health action for the prevention of suicide. 2012 [cited 2015 Jan 17]. Available from: http://www.who.int/mental_health/publications/prevention_suicide_2012/en/
- 2. Patton GC, Coffey C, Sawyer SM, Viner RM, Haller DM, Bose K, et al. Global patterns of mortality in young people: a systematic analysis of population health data. Lancet 2009;374(9693):881-892ArticlePubMed
- 3. In: Wassermand D, Wassermand C, editors. Oxford textbook of suicidology and suicide prevention: a global perspective. Oxford: Oxford University Press; 2009. p. 91-98
- 4. Organization for Economic Cooperation and Development. Health: key tables from OECD. 2012 [cited 2015 Jan 17]. Available from: http://www.oecd-ilibrary.org/social-issues-migration-health/health-key-tables-from-oecd_20758480Article
- 5. McIntosh JL. Suicide prevention in the elderly (age 65-99). Suicide Life Threat Behav 1995;25(1):180-192ArticlePubMed
- 6. Moscicki EK. Epidemiology of suicide. Int Psychogeriatr 1995;7(2):137-148ArticlePubMed
- 7. Jang YS, Jin JH. Epidemiology of suicide. 2012 [cited 2014 Dec 24]. Available from: https://www.kihasa.re.kr/html/jsp/share/download_forum.jsp?bid=21&aid=222&ano=140
- 8. Waern M, Rubenowitz E, Wilhelmson K. Predictors of suicide in the old elderly. Gerontology 2003;49(5):328-334ArticlePubMed
- 9. Choi YH, Kim SH. Suicide ideation and related factors according to depression in older adults. J Korean Gerontol Soc 2008;28(2):345-355. (Korean)
- 10. Bae JH, Um KW. Factors affecting suicide attempt of the elderly. J Korean Gerontol Soc 2009;29(4):1427-1444. (Korean)
- 11. Yoon HS, Park JY, Lim YO. Suicidal impulse caused by stress in Korea: focusing on mediational effects of existent spirituality, family support, and depression. Korean J Soc Welf Stud 2010;41(4):81-105. (Korean)Article
- 12. Kim CJ, Hwang JS. A study on the effects of senile disease and depression on the seniors’ ideation of suicide. J Korean Gerontol Soc 2008;28(3):425-442. (Korean)
- 13. Kim HS, Kim BS. A path analysis on suicidal ideation in the elderly. Korean J Couns Psychother 2007;19(3):801-818. (Korean)
- 14. Korea Centers for Disease Control and Prevention. The guide for using Community Health Survey raw data. Cheongju: Korea Centers for Disease Control and Prevention; 2012. p. 6-8 (Korean)
- 15. Bae SW, Shin WS. The factor structure of the CES-D Scale (the Center for Epidemiologic Studies-Depression Scale): an application of confirmatory factor analysis. Health Soc Sci 2005;18: 165-190. (Korean)
- 16. Kim HS. The elderly and deviant behavior. J Welf Aged 2000;10(1):25-45. (Korean)
- 17. Kim HC, Sohn YM. A study on the characteristics of elderly suicide and suicidal type. Korean J Psychol Soc Issues 2006;12(2):1-19. (Korean)
- 18. Park JE, Chung Y. The influencing factors on life-satisfaction and suicidal-ideation among elderly. Reg Dev Study 2005;10(1):39-59. (Korean)
- 19. Han SS, Kang SW, Yoo WK, Phee YG. A study of the determinants of suicidal ideation among the elderly in Korea. Health Soc Aff Rev 2009;29(1):192-212. (Korean)
- 20. Woo JP. Concept and comprehension for structural equation modeling. 1st ed. Seoul: Hanarae Press; 2012. p. 360-370 (Korean)
- 21. Conwell Y, Caine ED, Olsen K. Suicide and cancer in late life. Hosp Community Psychiatry 1990;41(12):1334-1339ArticlePubMed
- 22. Juurlink DN, Herrmann N, Szalai JP, Kopp A, Redelmeier DA. Medical illness and the risk of suicide in the elderly. Arch Intern Med 2004;164(11):1179-1184ArticlePubMed
- 23. Jeon HJ. Depression and suicide. J Korean Med Assoc 2011;54(4):370-375. (Korean)Article
- 24. Shin HG. Effects of Korean elder’s four major pains on suicidal thought mediated by depression: focused on Gyungrodang users. J Korean Gerontol Soc 2011;31(3):653-672. (Korean)
- 25. Kim HS, Kim BS. Verification of the structural relationship model of suicidal ideation to its related variables. Korean J Couns Psychol 2008;20(2):201-209. (Korean)
- 26. Kwon JD, Kim YJ, Um TY. Suicidal ideation among older adults who live alone with care services: a moderating effect of alcohol drinking in the relationship between previous suicidal attempts and suicidal ideation. J Welf Aged 2011;51: 297-320. (Korean)
REFERENCES
Figure & Data
References
Citations
Citations to this article as recorded by 

- Socioeconomic factors associated with suicidal behaviors in South Korea: systematic review on the current state of evidence
Nicolas Raschke, Amir Mohsenpour, Leona Aschentrup, Florian Fischer, Kamil J. Wrona
BMC Public Health.2022;[Epub] CrossRef - Suicidal Behavior Among Elderly Inpatients: its Relation to Functional Disability and Pain
Suzaily Wahab, Tien Yong Chua, Rosdinom Razali, Zanariah Mat Saher, Iman Hakimi Zamzam, Mohamad Adam Bujang
Psychology Research and Behavior Management.2022; Volume 15: 737. CrossRef - Parks and green areas and the risk for depression and suicidal indicators
Kyoung-bok Min, Hyun-Jin Kim, Hye-Jin Kim, Jin-young Min
International Journal of Public Health.2017; 62(6): 647. CrossRef - Prevalence and Predictive Factors of Depression in Community-Dwelling Older Adults in South Korea
Jae Soon Yoo, Sun Ju Chang, Hyun Sook Kim
Research and Theory for Nursing Practice.2016; 30(3): 200. CrossRef
 KSPM
KSPM


 PubReader
PubReader ePub Link
ePub Link Cite
Cite