Articles
- Page Path
- HOME > J Prev Med Public Health > Volume 50(2); 2017 > Article
-
Original Article
Income Differences in Smoking Prevalences in 245 Districts of South Korea: Patterns by Area Deprivation and Urbanity, 2008-2014 -
Ikhan Kim1
 , Jinwook Bahk2,3
, Jinwook Bahk2,3 , Tae-Ho Yoon4
, Tae-Ho Yoon4 , Sung-Cheol Yun5
, Sung-Cheol Yun5 , Young-Ho Khang1,2
, Young-Ho Khang1,2
-
Journal of Preventive Medicine and Public Health 2017;50(2):100-126.
DOI: https://doi.org/10.3961/jpmph.16.069
Published online: February 9, 2017
1Department of Health Policy and Management, Seoul National University College of Medicine, Seoul, Korea
2Institue of Health Policy and Management, Seoul National University Medical Research Center, Seoul, Korea
3Department of Public Health, Keimyung University, Daegu, Korea
4Department of Preventive and Occupational Medicine, Pusan National University School of Medicine, Yangsan, Korea
5Department of Clinical Epidemiology and Biostatistics, Asan Medical Center, University of Ulsan College of Medicine, Seoul, Korea
- Corresponding author: Young-Ho Khang, MD, PhD 103 Daehak-ro, Jongno-gu, Seoul 03080, Korea Tel: +82-2-740-8361, Fax: +82-2-743-2009 E-mail: yhkhang@snu.ac.kr
Copyright © 2017 The Korean Society for Preventive Medicine
This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/by-nc/4.0/) which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
ABSTRACT
-
Objectives
- The aim of this study was to measure income differences in smoking prevalence at the district level and to investigate correlations among area deprivation, smoking prevalence, and income differences in smoking prevalence, stratified by urbanity.
-
Methods
- Data were pooled from the Community Health Survey data of South Korea between 2008 and 2014. The age-standardized prevalence of smoking and its interquintile income differences were calculated. We conducted correlation analyses to investigate the association of the deprivation index with smoking prevalence and interquintile differences in smoking prevalence.
-
Results
- Across 245 districts, the median prevalence of smoking in men was 45.9% (95% confidence interval [CI], 43.4 to 48.5%), with an interquartile range (IQR) of 4.6% points. In women, the median prevalence was 3.0% (95% CI, 2.4 to 3.6%) and IQR was 1.6% points. The median interquintile difference in smoking prevalence was 7.4% points (95% CI, 1.6 to 13.2% points) in men and 2.7% points (95% CI, 0.5 to 4.9% points) in women. The correlation coefficients for the association between the deprivation index and smoking prevalence was 0.58, 0.15, -0.22 in metropolitan, urban, and rural areas, respectively, among men, and 0.54, -0.33, -0.43 among women. No meaningful correlation was found between area deprivation and interquintile difference in smoking prevalence. The correlation between smoking prevalence and interquintile difference in smoking prevalence was more evident in women than in men.
-
Conclusions
- This study provides evidence of geographical variations in smoking prevalence and interquintile difference in smoking prevalence. Neither smoking prevalence nor the deprivation index was closely correlated with interquintile income difference in smoking prevalence. Measuring inequalities in smoking prevalence is crucial to developing policies aimed at reducing inequalities in smoking.
- Tobacco smoking is an important risk factor for various health problems including cancers, cardiovascular diseases, and respiratory diseases [1]. Globally, approximately 5.8 million people died from tobacco smoking and 330 000 from exposure to second-hand smoke in 2013 [2]. Among the risk factors contributing to the global burden of disease, first and second-hand smoking rose from third place in 1990 to second place in 2013 [2].
- South Korea (hereafter Korea) is also facing a smoking epidemic. The smoking prevalence of men has decreased from 66.3% in 1998 to 42.1% in 2013 by tobacco control activities at the government and non-government organizational levels [3]. However, among the Organization for Economic Cooperation and Development countries, smoking rate among men aged 15 or older was highest in Korea in 2013 [4]. According to the Global Burden of Disease study 2013, tobacco smoking was the greatest contributor to the burden of disease in Korea [2]. Smoking is also one of the primary causes of health inequality in Korea. Both men and women with a lower socioeconomic status have been shown to have a higher age-standardized smoking prevalence than their counterparts [5-7]. A prior study showed that the size of the absolute inequalities in all-cause and cardiovascular mortality could be greatly reduced by eradicating smoking [8].
- The reduction of socioeconomic inequality in smoking prevalence has been a policy agenda in the Korean government’s health promotion policy. The focus has been on reducing the differences according to income levels. Reducing smoking prevalence differences between income levels was first set as a health equity target in the ‘National Health Plan 2010’ in 2005 [9]. In 2010, the ‘National Health Plan 2020’ also set targets to reduce differences in smoking prevalence among income levels as well as geographical areas (rural vs. urban areas) [10], and these targets were maintained in 2015 [11]. Some provincial municipalities (such as Seoul) in Korea have monitored socioeconomic differences in smoking and set goals to reduce such differences [12,13]. However, it is difficult to find cases where local district governments (si, gun, gu) have set the reduction of socioeconomic inequality in smoking prevalence as a goal in Korea. One main reason behind this is that the socioeconomic differences in smoking prevalence are not being monitored at the local district government level.
- Although it may be possible to obtain the smoking prevalence for a si, gun, or gu using Community Health Survey (CHS) data in Korea, the sample size of one year data is insufficient to calculate the differences in smoking prevalence according to socioeconomic position indicators such as income level. However, by pooling many years of CHS data, it would be possible to reliably estimate the income differences in smoking prevalence at the level of districts (si, gun, and gu).
- The magnitude of the income differences in smoking prevalence might vary across the local districts. Explaining the geographical variation in the size of inequalities in smoking prevalence is an interesting line of research. In particular, since a previous study showed that the area deprivation index and smoking prevalence (especially for women) are closely related [6], determining the relationship between the area deprivation index and the income differences in smoking prevalence would be warranted. However, since some studies indicated that the area deprivation index was not a strong indicator of health status for Korea’s rural areas [14,15], the relationships among the area deprivation index, smoking prevalence, and income differences in smoking prevalence should be clarified in both rural and urban areas.
- In this study, we employed pooled data of CHS between 2008 and 2014 and examined the income differences in smoking prevalence at the local administrative district level in Korea. We also explored the relationships among the area deprivation index, smoking prevalence, and income differences in smoking prevalence in both rural and urban areas.
INTRODUCTION
- Data and Administrative Districts
- This study was approved by the Seoul National University Hospital Institutional Review Board. The data came from the CHS raw data, with the compilation of seven years of data (2008-2014). The CHS is a repeated cross-sectional study that has been conducted annually since 2008 on about 900 residents for each of 252 districts. Subjects of the survey were household members who were 19 years old or older. All surveys were conducted with a face-to-face computer-assisted personal interviewing method. This study utilized 1 594 873 of the 1 595 410 total individuals who participated in the survey from 2008 to 2014 as the subjects of analysis, after excluding 537 individuals who had missing values for smoking status.
- The administrative districts of the CHS was classified into 17 metropolitan cities and 252 districts according to the 2015 governmental administrative classification. However, in consideration of the changes in administrative units from 2008 to 2014, the administrative districts were reclassified into 245 districts to maintain the consistency of geographical classification over the study periods. In the case of Jeonju-si, although it is currently divided into Wansan-gu and Deokjin-gu, they were combined into a single Jeonju-si. Tonghap Changwon-si was divided into Uichang-gu, Seongsan-gu, Masanhoewon-gu, Masanhappo-gu, and Jinhae-gu when Changwon-si, Masan-si, and Jinhae-si were combined in 2010. Uichang-gu and Seongsan-gu were combined as Changwon and Masanhoewon-gu and Masanhappo-gu were also combined as Masan.
- Cheongju-si and Chungwon-gun were combined in 2014 and divided into Sangdang-gu, Heungdeok-gu, Seowon-gu, and Cheongwon-gu. However, they were all combined and analyzed in this study as Cheongju-si. In 2008, Cheonan-si created two new districts, Dongnam-gu and Seobuk-gu. However, they were combined as Cheonan-si and analyzed as one unit in this paper. Yeongi-gun was integrated into Sejong Special Autonomous City from July 1 in 2012, and hence was not considered as a separate unit of analysis. For Sejong Special Autonomous City, the analysis was conducted on the data from 2012 to 2014, and since the area deprivation index was based on 2010 census data, Sejong Special Autonomous City was excluded from the analysis related to the area deprivation index. The urbanity was categorized based on the administrative districts with “si” as urban area, “gu” as metropolitan area, and “gun” as rural area.
- Smoking
- Smoking prevalence was calculated based on the responses to the current smoking status question. Current smokers were defined as respondents who smoked five or more packs (100 or more cigarettes) of cigarettes in their lifetime and replied “yes” to the question “do you smoke currently” (2008), or replied “smokes daily” or “occasionally smokes” (2009 and beyond).
- Income
- The “equivalized annual household income” using the equivalence scale was used for income [17]. The method used for prior studies [7,18] was used, with the following formula:
- where Y=annual household income, A=number of adults in household, B=number of household members below the age of 19, β, V=equivalence scale (β=1, V=0.5)
- Unlike those used from 2008 to 2013, the household income questions in the 2014 CHS shifted to a categorical format for monthly household income ([1] under 500 000 won, [2] 500 000 to 1 000 000 won, [3] 1 000 000 to 2 000 000 won, [4] 2 000 000 to 3 000 000 won, [5] 3 000 000 to 4 000 000 won, [6] 4 000 000 to 5 000 000 won, [7] 5 000 000 to 6 000 000 won, [8] over 6 000 000 won). Hence, in this paper, the median of each of the ranges was taken as the monthly household income, which was then used to calculate the annual household income. For example, those who replied with “500 000 to 1 000 000 won” would be considered as having a monthly household income of 750 000 won and those who replied “over 6 000 000 won” were considered to have a monthly household income of 6 500 000 won.
- According to a Household Income and Expenditure Survey in Korea [19], the 80th percentile monthly income of a household of at least two individuals in 2014 was 5 975 453 won. This means that those who responded as earning “over 6 000 000 won” were part of the uppermost quintile, which indicates that the estimation of 6 500 000 won as the monthly income would not be inappropriate. Despite the differences in questions on income in the 2014 CHS data, we used the 2014 data in order to present stable estimates for the income difference in smoking prevalence. In order to take into account the differences in real income from 2008 to 2014, the annual household income was adjusted by consumer price index (CPI) with 2010 as reference year. For example, the 2011 CPI modified household income was calculated by taking the 2011 household income and multiplying the 2010 and 2011 CPI ratio (100/104).
- When compiling the CHS data from 2008 to 2014, 111 499 respondents (6.7% of total subjects) were missing for household income information. However, to calculate representative smoking prevalences according to income levels for each district, the entire samples were used. The missing values for income were imputed with use of the following variables: CPI adjusted household income, gender, age, number of household members, education level, and occupation. With these imputed income, the income quintiles of each district were calculated according to gender and age groups.
- Because the quintiles were created for each si, gun, and gu, the income quintile in this study could be considered as relative income within individual district (si, gun, and gu). The reason relative income data was used is because the smoking prevalence of the income quintiles in each si, gun, and gu is a meaningful indicator of equity for each district.
- The Korean National Health and Nutrition Examination Survey (KNHANES) data contains information on income quartiles rather than income quintiles considering small sample sizes in certain age groups, and have presented information on smoking prevalence by income quintile. However, we used the income quintile, which is more widely used for inequality research.
- Area Deprivation Index
- The area deprivation index is a summary measure that is used to indicate the material and social deprivation levels of a geographical area, and consists of a number of standardized and weighted variables [20]. Substantial research has proven that the area deprivation index can be useful for uncovering geographical differences in health [21]. Such a relationship between the area deprivation index and health indicators has also been reported in Korea [6,22]. The area deprivation index in this study was calculated based on the 2010 population census data in Korea.
- A total of nine variables were used for construction of the area deprivation index: proportion of people living alone, proportion of households with a women household head, proportion of households without a car, proportion of households not living in an apartment, proportion of households living below the minimum housing standard, proportion of people aged 30-64 with no high school diploma, proportion of people in households with economically active heads aged 15-64 who are employed in manual labor, proportion of population aged 65 or over, and proportion of separated, divorced or widowed among people aged ≥15 years. Each of the variables was standardized using a Z-score, then combined to calculate the area deprivation index [22]. The median of the area deprivation index was -1.6, the minimum (the lowest deprivation) was -17.7, the maximum (the highest deprivation) was 16.8, and the standard deviation (SD) was 7.8.
- Statistical Analysis
- After combining seven years (2008-2014) of CHS data, income quintile data (5 groups) were produced using CPI-adjusted equivalized household annual income data for gender (men or women) and six age groups (19-29, 30-39, 40-49, 50-59, 60-69, above 70). Cumulative proportions regarding the equivalized income were used to identify the nearest quintile points in income. Then, population size (denominator) and number of smokers (numerator) for each of 14 700 numerator denominator groups from 245 si, gun, and gu were determined, and these data were used for calculating the age-standardized smoking prevalence according to gender, districts (si, gun, gu), and income level.
- Sample weights were considered in the analysis. The original sample weights provided by the CHS data were assigned to represent the entire population of the district. Thus, the variation between individual weights was large, and in the case of subgroup analysis involving respondents with a large sample weight, this would result in a biased estimate. In this study, we recalculated sample weights. The sum of the weights in the district was recalculated to be equal to the total number of respondents in each year. The average weight of respondents was adjusted to be one.
- For women, in 970 groups out of 7350 numberator-denominator groups, the number of smokers considering sampling weight was found to be zero. For such cases, the age-standardized rate was calculated by substituting 0.01 for 0 in the numerator to avoid distorting the estimation of the age-standardized rate. The standard population used for the age-standardized rate was the 2010 Korean population census data. This study also provided 95% confidence intervals (CI) of the income differences in smoking prevalence. The 95% CIs were derived using the following formula:
- Where “Lower”=minimum of the 95% CI, “Upper”=maximum of the 95% CI, “Diff”=difference in the age-standardized smoking prevalence between the upper and lower 20% of income levels.
- P1=age-standardized smoking prevalence of the highest quintile income level, P2=age-standardized smoking prevalence of the lowest quintile income level, N1=population of the highest quintile income level, N2=population of the lowest quintile income level.
- The health inequality between income levels can be presented with different inequality measures such as the prevalence ratio, the relative index of inequality, and the absolute index of inequality. This study used the absolute prevalence difference in smoking between the uppermost quintile and lowermost quintile of the income groups as the measure for health inequality. This was because the ‘National Health Plan 2020’ has employed the absolute difference in smoking prevalence between the upper and lower tiers of income levels as an equity target indicator [10,11]. In addition, interquintile income difference in smoking prevalence also has the benefit of being relatively easier for the layperson to understand compared to the prevalence ratio, relative index of inequality, or absolute index of inequality.
- We conducted correlation analyses between the age-standardized smoking prevalence and the area deprivation index, and also between the income differences in smoking prevalence in districts (si, gun, and gu) and the area deprivation index. Separate analyses were conducted for urban and rural areas. SAS version 9.4 (SAS Institute Inc., Cary, NC, USA) was used for the analysis.
METHODS
- Table 1 shows the characteristics of the study subjects. Of the 1 594 873 individuals who participated in the CHS, 45.4% were men and 54.6% were women. The average age of the respondents was 46.8 years in metropolitan areas, 50.0 years in urban areas, and 56.9 years in rural areas. The weighted mean age was highest in the rural areas, followed by urban areas, with metropolitan areas the youngest. A total of 315 720 men smoked (smoking prevalence, 43.6%), while 28 830 women (smoking prevalence, 3.3%) smoked. The age-standardized smoking prevalence were 45.8% for men (95% CI, 45.6 to 45.9%) and 3.2% for women (95% CI, 3.1 to 3.2%).
- The age-standardized smoking prevalence for men was lower in the metropolitan areas compared to the urban and rural areas, while that of women was lower in rural areas than metropolitan and urban areas. The area deprivation index had an average of 0.0 and a SD of 7.8. The metropolitan areas had an average deprivation index of -5.0 (SD, 4.4), the urban areas, -2.6 (SD, 5.7), and the rural areas, 7.9 (SD, 5.8), indicating that rural areas had relatively higher deprivation levels.
- As seen in Table 2, the median age-standardized smoking prevalence for men in 245 districts was 45.9% (95% CI, 43.4 to 48.5%) in Gangwon-do Chuncheon-si and five other districts, while the minimum was 31.4% (95% CI, 29.3 to 33.5%) in Gyeonggi-do Gwacheon-si, and the maximum was 56.1% (95% CI, 53.3 to 58.8%) in Gangwon-do Taebaek-si; the IQR was 4.6% points (p), and the SD was 3.6%p. For women, the median was 3.0% (95% CI, 2.5 to 3.6%) in Gyeongsangbuk-do Andong-si and nine other districts, the minimum was 0.8% (95% CI, 0.5 to 1.1%) in Jeollanam-do Goheung-gun and one other district, and the maximum was 7.4% (95% CI, 6.5 to 8.3%) in Gyeonggi-do Dongducheon-si. The IQR was 1.6%p and the SD was 1.1%p.
- When considering both the districts and the income levels, the lowest age-standardized men smoking prevalence was in the highest income group in Gyeonggi-do Seongnam-si Bundang-gu, at 24.6% (95% CI, 20.6 to 28.7%), while the highest smoking prevalence was in the lowest income level in Gangwon-do Taebaek-si, at 59.8% (95% CI, 53.6 to 65.9%). The difference between the two was 35.2%p. For women, the highest income group of Jeollanam-do Jangseong-gun and two other gun had the lowest smoking prevalence, at 0.2% (95% CI, 0.0 to 0.4%), and the lowest income group of Gyeonggi-do Dongducheon-si had the highest smoking prevalence, at 13.0% (95% CI, 10.2 to 15.8%). The difference between the two was 12.8%p. The median value of the difference between the men age-standardized smoking prevalence of the uppermost quintile and the lowermost quintile income level was in Gyeonggi-do Bucheon-si Sosa-gu and three other districts, at 7.4%p (95% CI, 1.6 to 13.2%p). The minimum was in Gyeonggi-do Uijeongbu-si, at -3.7%p (95% CI, -9.7 to 2.3%p), and the maximum was in Gyeongsangbuk-do Uljin-gun, at 20.2%p (95% CI, 14.4 to 26.0%p). The IQR was 5.9%p, and the SD was 4.1%p.
- The median value of the difference between women age-standardized smoking prevalence was in Gangwon-do Jeongseon-gun and eight other districts, with a value of 2.7%p (95% CI, 0.5 to 4.9%p), the minimum was in Incheon Metropolitan City Ongjin-gun, at -1.4%p (95% CI: -3.8 to1.0%p), and the maximum was in Gyeonggi-do Dongducheon-si, at 9.5%p (95% CI: 6.5 to 12.5%p). The IQR was 2.0%p and the SD was 1.6%p. The women age-standardized smoking prevalence and the income difference in the age-standardized smoking prevalence were the highest in Gyeonggi-do Dongducheon-si. Of the 245 districts, 236 districts had a difference in men smoking prevalence between income groups greater than 0%p (i.e., with the lower income group having a higher smoking prevalence than the higher income group), while in 239 districts, this was the case for women. When considering the 95% CI, 163 districts out of 245 had a men smoking prevalence of the lowest quintile income level that was significantly greater than that of the uppermost quintile income level, whereas this was the case for women in 173 districts. There were no districts where the uppermost income quintile had a significantly greater smoking prevalence than the lowest quintile.
- Supplemental Tables 1 and 2 show the 10 districts where the age-standardized smoking prevalence and the income difference in smoking prevalence were the greatest or the least. The men age-standardized smoking prevalence was high in Gangwon-do Taebaek-si (56.1%), Gyeonggi-do Pocheon-si (52.7%), Gangwon-do Jeongseon-gun (52.3%), and low in Gyeonggi-do Gwachon-si (31.4%), Gyeonggi-do Seongnam-si Bundang-gu (33.0%), and Seoul Seocho-gu (34.4%). For women, the age-standardized smoking prevalence was high in Gyeonggi-do Dongducheon-si (7.4%), Incheon Metropolitan City Jung-gu (5.9%), and Gyeonggi-do Bucheon-si Ojeong-gu (5.7%), and was low in Jeollanam-do Goheung-gun (0.8%), Jeollanam-do Muan-gun (0.8%), and Jeollanam-do Boseong-gun (1.0%).
- The income difference in age-standardized smoking prevalence for men was large in Gyeongsangbuk-do Uljin-gun (20.2%p), Gyeonggi-do Anseong-si (18.0%p), and Seoul Mapo-gu (17.0%p), and was small in Gyeonggi-do Uijungbu-si (-3.7%p), Gangwon-do Inje-gun (-2.9%p), and Jeollanam-do Jindo-gun (-2.5%p). The income difference in age-standardized smoking prevalence for women was high in Gyeonggi-do Dongducheon-si (9.5%p), Gyeonggi-do Ansan-si Sangrok-gu (6.7%p), and Gyeongsangnam-do Tongyeong-si (6.7%p), and low in Incheon Metropolitan City Ongjin-gun (-1.4%p), Gyeongsangbuk-do Uljin-gun (-1.0%p), and Gyeongsangbuk-do Ulleung-gun (-0.9%p). The men and women age-standardized smoking prevalence and the differences in smoking prevalence between income quintiles for 245 si, gun, and gu can be seen in Supplemental Tables 3.
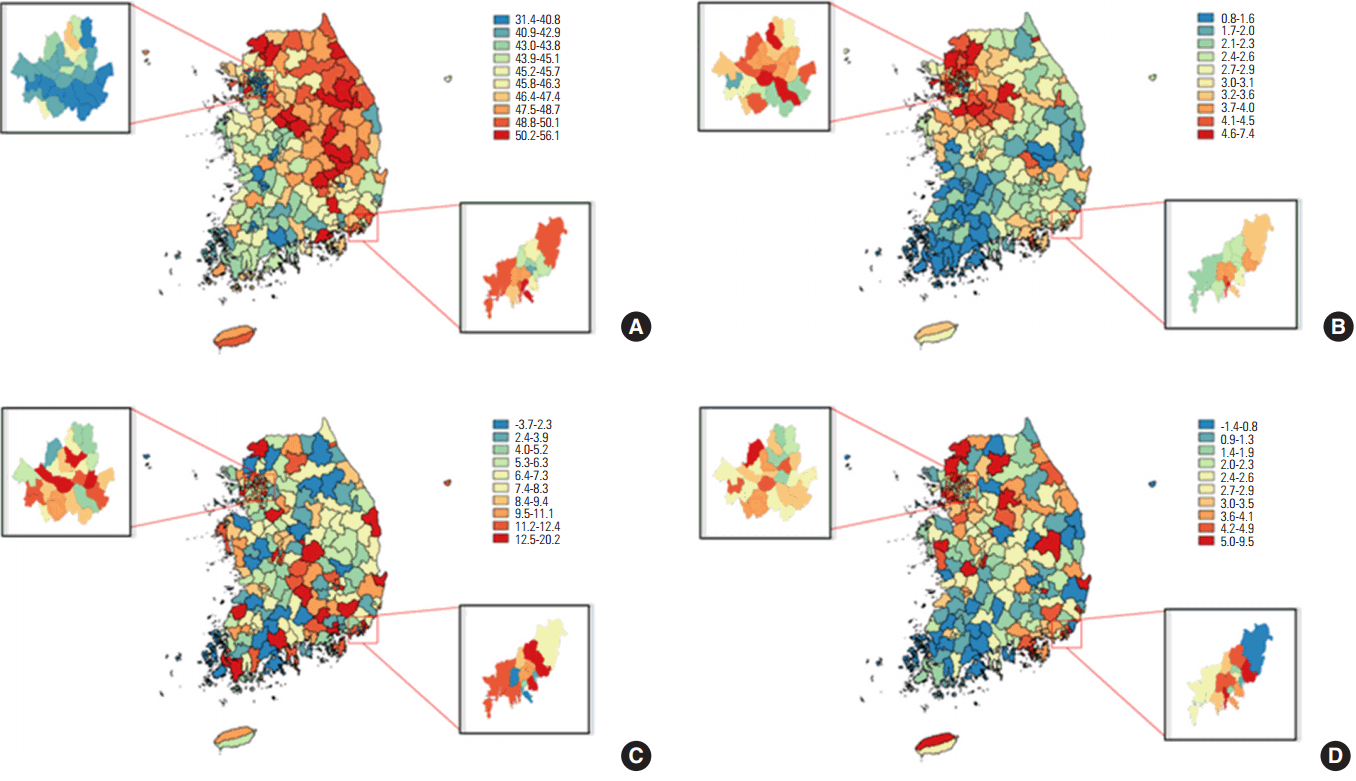
- Figure 1 (A and B) is shown the age-standardized smoking prevalence for individual si, gun, and gu. For men, parts of the northeast and the southeast of the country are colored in red, indicating a high smoking prevalence, while women showed a high smoking prevalence around the capital city, Seoul. The men smoking prevalence in Seoul was low overall, but the Gangbuk districts were relatively higher than rest of the districts within Seoul. For women in Seoul, a high smoking prevalence was seen in Gwangjin-gu, Yongsan-gu, and Mapo-gu. For men in Busan, the smoking prevalence in western areas, such as Dong-gu and Busanjin-gu, was higher than that of the eastern areas such as Haeundae-gu. For women, part of the western area, Haeundae-gu, and Gijang-gun districts showed a higher smoking prevalence relative to other districts within Busan.
- Figure 1 (C and D) shows the smoking prevalence inequality amongst income levels for each si, gun, and gu based on gender. For men, the differences in the southeastern districts and the northeastern districts were relatively large, while for women, the areas around the capital and some of the central districts had relatively large differences. In Seoul, there was a large difference in Mapo-gu, Yongsan-gu, and Gwangjin-gu districts for men, and in Yongsan-gu and Dongdaemun-gu for women. In Busan, men had relatively large gaps in all areas excluding Saha-gu, Sasang-gu, and Buk-gu, while women had large gaps in the Haeundae-gu, Jung-gu, and Seo-gu areas.
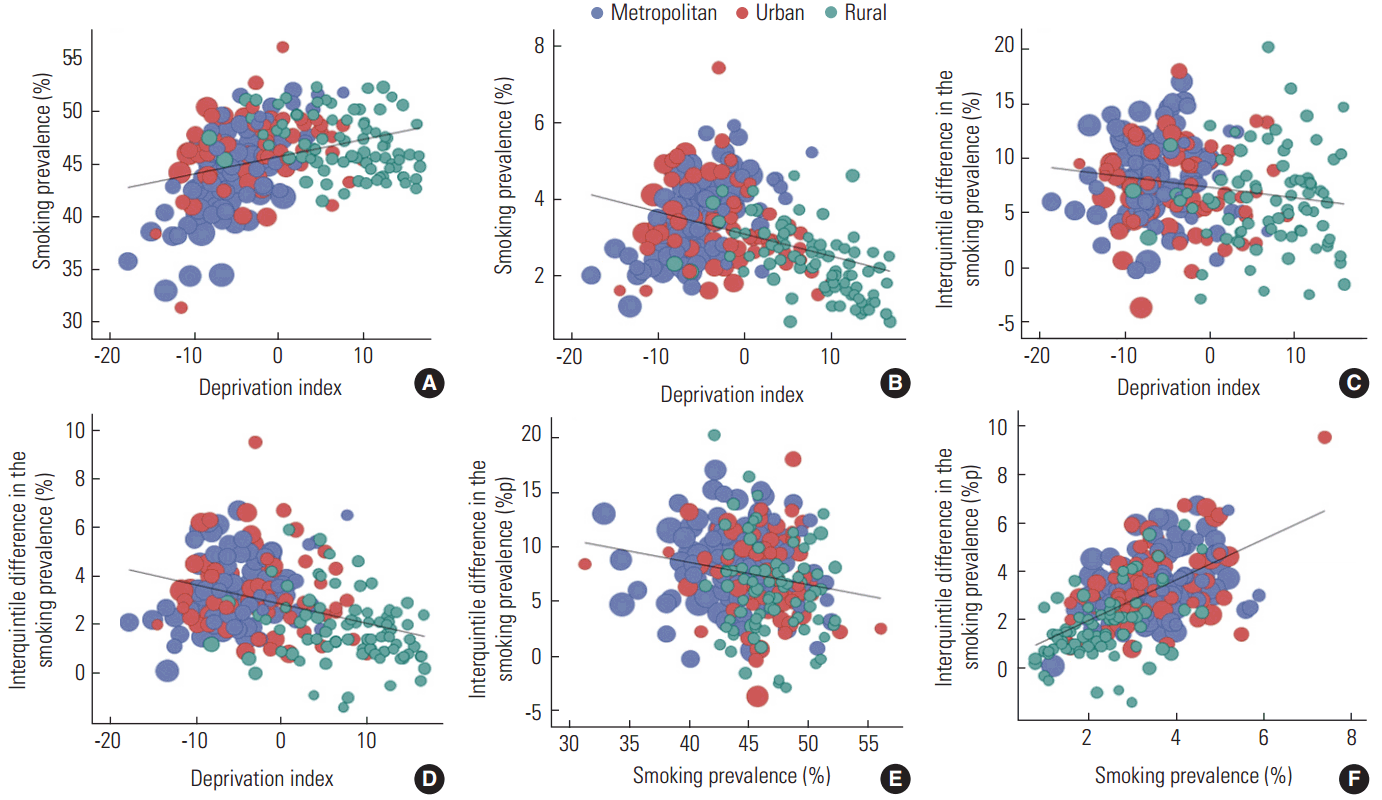
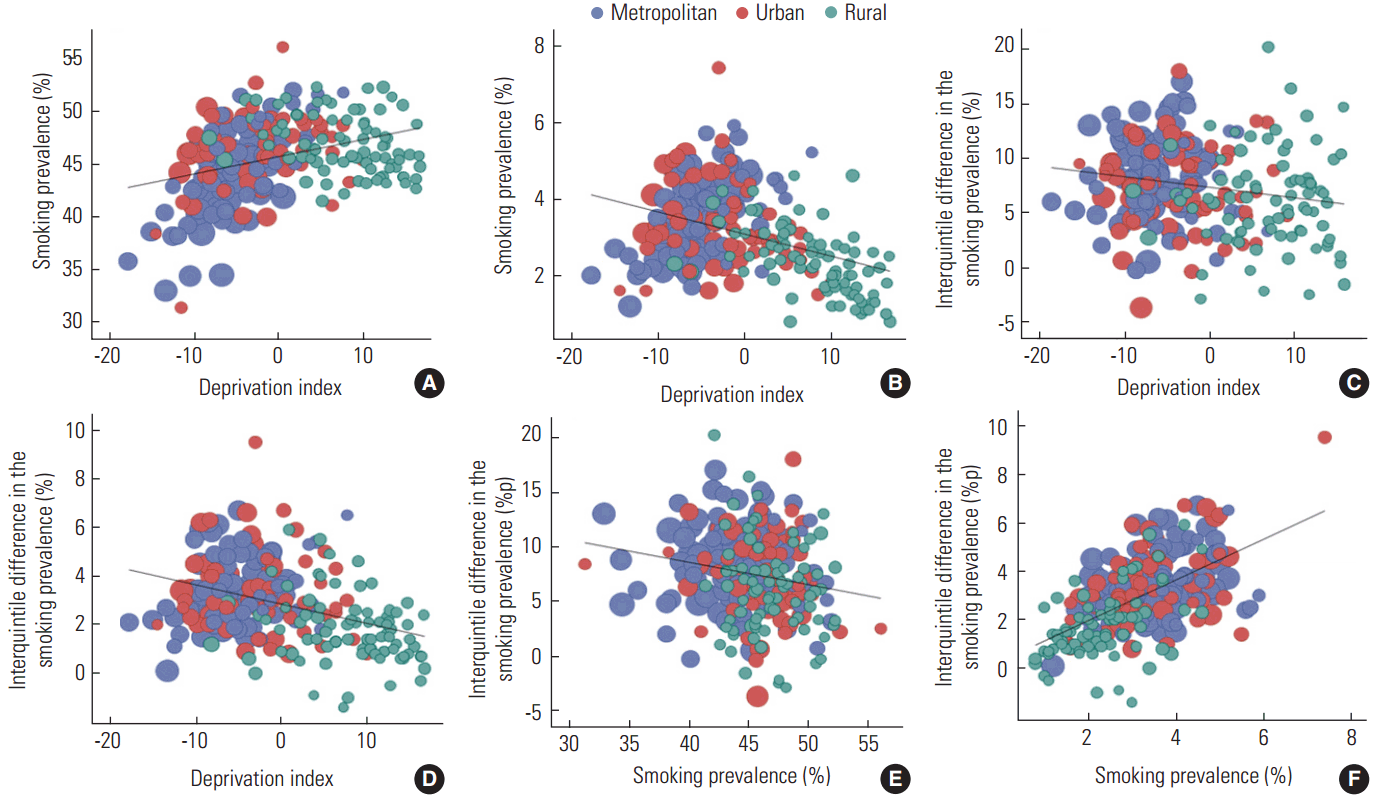
- Table 3 presents the correlation coefficients of the area deprivation index with overall smoking prevalence, smoking prevalence of the highest and lowest income quintiles, and interquintile income differences in smoking prevalence. Table 3 also shows the correlation coefficients between smoking prevalence and the income difference in smoking prevalence. For men, the correlation coefficient between the area deprivation index and the age-standardized smoking prevalence was 0.58 (p<0.001) for metropolitan areas. However, the coefficient was drastically lower in urban areas, at 0.15 (p=0.24), and ran in the opposite direction in rural areas, at -0.22 (p=0.05). For women, the coefficient was 0.54 (p<0.001) for metropolitan areas, but was -0.33 (p=0.008) and -0.43 (p<0.001) for urban and rural areas, respectively.
- The correlation coefficients of the area deprivation index with smoking prevalence in the highest and lowest income quintiles showed a similar trend. However, the correlation coefficient for women in urban areas showed a relatively low value (the correlation coefficient of the highest income quintile, 0.33; p<0.001; the correlation coefficient of the lowest income quintile, 0.40; p<0.001). The correlation coefficient between the area deprivation index and the income difference in age-standardized smoking prevalence was, for men, 0.04 (p=0.70) in metropolitan areas, 0.08 (p=0.03) in urban areas, and -0.01 (p=0.94) in rural areas. For women, the correlation coefficient was 0.22 (p=0.03) in metropolitan areas, -0.14 (p=0.28) in urban areas, and -0.16 (p=0.15) in rural areas. The correlation coefficient between the age-standardized smoking prevalence and the income difference in the age-standardized smoking prevalence was relatively small with values, for men, of -0.03 (p=0.77) for metropolitan areas, -0.16 (p=0.21) for urban areas, and -0.07 (p=0.54) for rural areas. However, for women, the coefficients were relatively large, at 0.38 (p<0.001), and 0.48 (p<0.001), 0.39 (p<0.001), respectively. Figure 2 shows the coefficients graphically, with sample weights based on the population of the individual si, gun, gu taken into account.
- Supplemental Figure 1 presents separate analyses for rural and urban areas. Results showed that for men, the patterns of association between smoking prevalence and the area deprivation index were similar for upper and lower income quintiles. However, for women, the patterns varied with urbanity. In metropolitan cities, the magnitude of the positive association between smoking prevalence and the area deprivation index tended to be larger in the lower 20% income group than that in the uppermost income quintile. In rural areas, however, the reverse was true with the lowest income quintile recording a larger decrease in smoking prevalence as the area deprivation index increased. Meanwhile, in all three areas, the interaction between the deprivation index and the income level variations were not statistically significant.
RESULTS
- This study demonstrates the magnitude of the inequality in the age-standardized smoking prevalence and the income difference in smoking prevalence for each si, gun, and gu in Korea. The smoking prevalences of each district have been published annually by the Korea Centers for Disease Control and Prevention. However, this study is unique in that no other study has demonstrated the magnitude of the smoking prevalence inequality by income level for each district; nor has the inequality been examined based on the area deprivation index and urbanity. The results of this study should be useful as basic data to inform the development of public health centers’s policies and programs for equity in smoking prevalence in each district. Furthermore, local governments might well compare the data on their own area with nationwide data to establish an equity target in smoking prevalence.
- The results of this study presented the age-standardized smoking prevalence was higher for lower income groups in most districts. This was true for both men and women. Of the 245 districts, 96.3% (236 districts) in men and 97.6% (239 districts) in women had a higher smoking prevalence in the lowest income quintile than in the highest quintile. In other words, income differences in smoking prevalence was observed in the overwhelming majority of districts. In addition, in those few districts where the smoking prevalence of the uppermost income quintile was higher than that of the lowest quintile, the difference was not statistically significant.
- Moreover, the income differences in smoking prevalence were statistically significant in 66.5% (163 districts) of total 245 districts in men and 70.6% (173 districts) of total districts in women. These results demonstrate that pro-rich smoking inequality is prevalent for both men and women in Korea. Although a few districts (9 for men and 5 for women) had the income difference in smoking prevalence reversed (but statistically insignificant), this might be attributed to small sample size for each income group, sub-optimal accuracy of income data, and stochastic chance findings.
- Analysis results showed that the magnitude of income differences in smoking prevalence in the 245 districts was similar to or greater than the magnitude of the variations in smoking prevalence among those districts. The difference between the maximum (Gangwon-do Taebaek-si) and the minimum (Gyeonggi-do Gwacheon-si) men smoking prevalence was 24.7%p, while the difference between the maximum (Seoul Mapo-gu) and minimum (Gyeonggi-do Uijeongbu-si) magnitude of income differences in men smoking prevalence was 23.9%p. The SD of men smoking prevalence in the 245 districts was 3.6%p, while that of the magnitude of income differences in men smoking prevalence was 4.1%p.
- The difference between the maximum (Gyeonggi-do Dongducheon-si) and minimum (Jeollanam-do Goheung-gun) women smoking prevalence was 6.6%p, while the difference between the maximum (Gyeonggi-do Dongducheon-si) and minimum (Incheon-si Ongjin-gun) magnitude of income differences in women smoking prevalence was 10.9%p. The SD for women smoking prevalence for the 245 districts was 1.1%p, while that of the magnitude of income differences in smoking prevalence was 1.6%p. Further research is required to explain the variations in smoking prevalence among districts and the variations in the magnitude of inequality in smoking prevalence between districts.
- Analysis results showed discrepancies between the districts with high age-standardized smoking prevalence and those with high inequality in smoking prevalence. This is particularly the case for men. For men, the correlation between the age-standardized smoking prevalence and the magnitude of income differences in smoking prevalence was not evident, while the correlation coefficient for women was around 0.4 to 0.5. In addition, very little correlation was found between the area deprivation index and the income difference in smoking prevalence. These results indicate that measures such as smoking prevalence and area deprivation index are not very useful in estimating the magnitude of inequality in smoking prevalence.
- This also demonstrates that promoting policies to reduce smoking prevalence inequality between income levels simply based on the information on the smoking rate and the deprivation level may not be appropriate at the district level. The results showed that to develop a policy to reduce the magnitude of inequality in smoking prevalence, an effort should be exercised to directly measure the magnitude of the smoking inequality. Taking into account that it is difficult to measure the inequality in smoking prevalence according to income with use of the CHS data at the level of districts annually or in a short period of time (for example biennially) due to limitations in sample size, there is a need to adopt a monitoring method that utilizes the health examination data of the national health insurance database.
- According to the descriptive model for smoking epidemic in developed countries [23], either no difference in smoking prevalence by socioeconomic status or higher smoking prevalence in the upper social class appears when smoking prevalence increases, while the higher smoking prevalence can be observed in lower social classes when a smoking epidemic occurs and then smoking prevalence decreases. In this study, higher smoking prevalence was generally observed in lower income groups in both gender. However, the smoking prevalence based on the area deprivation index, which can be considered a socioeconomic indicator of geographical areas, showed different patterns according to urbanity. In metropolitan areas, smoking prevalence increased as the area deprivation index increased, but the opposite was the case in rural areas.
- This trend was prevalent in women rather than men. These trends in metropolitan areas can be attributed to both the compositional effect and the contextual effect. Factors such as easily accessible cigarette stores [24], repeated exposure to cigarette advertisements and tobacco industry promotions [25,26], and the slower establishment of non-smoking buildings due to the smaller size of buildings and restaurants [27] might have affected the relatively greater smoking prevalence in districts with higher deprivation in metropolitan areas. In addition, these districts might well have a relatively higher composition of individuals with lower socioeconomic statuses, such as education, occupation, and income. According to a previous Korean study [28], which observed the relationship between socioeconomic position indicators at the level of districts and smoking prevalence, inequality in smoking prevalence due to individual socioeconomic position indicators (education, occupation, and income) was clearly seen in both men and women.
- This prior study [28] also revealed that the smoking prevalence according to the district’s socioeconomic indicators were not clear for women. It has been posited that cultural factors associated with women smoking might have affected the smoking prevalence patterns based on a district’s indicators. There exists the possibility that societal intolerance towards women smoking and cultural differences might have lowered women smoking prevalence in si and gun areas with high area deprivation indices. A study conducted by Cho et al. [29], which reported differences in smoking prevalence based on occupational categories, indicated that women in the service sector in Korea have a higher smoking prevalence than women with other occupations. Hence, the lack of women in the service sector in rural areas with high area deprivation levels might also explain the phenomena. However, the negative relationship between the area deprivation index and smoking prevalence in rural areas, which also appears for men, cannot be easily explained by these factors.
- Supplemental Figure 2 shows the results on the relationship between age-standardized smoking prevalence and the area deprivation index that was explored to explain the relationship between the area deprivation index and smoking prevalence for men in rural areas. According to the results, a strong negative correlation was observed in the 19-29 age group. It is interesting that 19 to 29-year-old men in rural areas with a high area deprivation index had a relatively low smoking prevalence. Supplemental Figure 3 shows the number of people per convenience store based on the area deprivation index for metropolitan, urban, and rural areas. In Supplemental Figure 3, the number of people per convenience store increased steeply in rural areas as the area deprivation increased [30].
- Because advertisement of tobacco products through mass media has been restricted in Korea, tobacco companies have reportedly focused on promotions through displays and posters in convenience stores, image marketing, and corporate social responsibility activieis [31]. Internal documents from tobacco companies have revealed that these types of sales promotion activities have targeted the 18-24 age group [32,33]. Considering these factors, it may be possible that the reason the smoking prevalence of people in their 20s decreased as the area deprivation index in rural areas decreased is because of their limited exposure to the promotion strategies of the tobacco industry.
- According to this study, for women, as the smoking prevalence increased, the difference in smoking prevalence between income levels also increased. This is probably because the smoking prevalence of women in Korea was low; hence an increase in smoking prevalence also was associated with an increase in the absolute smoking prevalence differences [34].
- This study has several limitations. Firstly, the women smoking prevalence of 3.4% measured in this study is lower than the prior analysis results utilizing the KNHANES data [3]. According to a prior study by Jung-Choi et al. [35] using the 2008 KNHANES data, the smoking prevalence estimated from urinary cotinine tests was higher than the self-reported smoking prevalence by 5.3%p in men and 8.0%p in women. In particular, women who live with a spouse or parents or live in a gun district had a tendency to underestimate their smoking behavior. These findings suggest that self-reported smoking in women may be subject to bias. In particular, the women smoking from the CHS was likely to be underreported because women were surveyed in households with family members, unlike KNHANES where interviews on smoking behaviors were conducted in separation from household members. Secondly, the income information in the CHS was changed to a categorical response from 2014. In most districts, the percentage of the people responding with ‘more than 6 000 000 won’ was less than 20%, hence assuming these individuals as the uppermost income level would be appropriate. However, in Seoul Gangnam-gu, Seocho-gu, Songpa-gu, the percentage of respondents was 38.4, 37.1, and 25.1%, respectively. Therefore, there is a possibility that the calculation of the income quintiles for household with more than 6 000 000 won would be inaccurate for some affluent districts.
- Despite these limitations, this study is notable in that it reported the size of the income differences in smoking prevalence for each si, gun, and gu throughout the country. Furthermore, it also presented the relationship between the inequality in the smoking prevalence and area deprivation levels in metropolitan, urban, and rural areas.
- In summary, this study revealed a large difference in not only smoking prevalences, but also the size of inequality in smoking prevalence among 245 districts in Korea. Districts with a high age-standardized smoking prevalence did not necessarily have a large inequality in smoking prevalence. In addition, the correlation between the area deprivation index and smoking prevalence was different for metropolitan, urban, and rural areas. The relationship between the area deprivation index and size of the smoking prevalence inequality was not evident.
- These results suggest that to develop a policy or a target for equity in smoking prevalence in si, gun, and gu areas of Korea, an effort should be exercised to directly measure the magnitude of the inequality in smoking prevalence rather than to assume the magnitude based on overall smoking prevalence or area deprivation indices. Further research to explain the geographical variations in smoking prevalence and the size of inequality in smoking prevalence along with research to examine the time trends in smoking prevalence inequality for each si, gun, and gu is needed.
DISCUSSION
ACKNOWLEDGEMENTS
-
CONFLICT OF INTEREST
The authors have no conflicts of interest associated with the material presented in this paper.
Notes
SUPPLEMENTAL MATERIAL
Supplemental Table 1.
Supplemental Table 2.
Supplemental Table 3.
Supplemental Figure 1.
Supplemental Figure 2.
Supplemental Figure 3.

| Overall | Metropolitan1 | Urban1 | Rural1 | |
|---|---|---|---|---|
| No. of districts | 245 | 98 | 65 | 82 |
| Mean (SD) of area deprivation index2 | 0.0 (7.8) | -5.0 (4.4) | -2.6 (5.7) | 7.9 (5.8) |
| No. of study subjects | 1 594 873 | 524 696 | 368 965 | 422 670 |
| Men | 724 697 (45.4) | 288 911 (45.5) | 204 324 (45.9) | 231 462 (45.0) |
| Women | 870 176 (54.6) | 346 259 (54.5) | 241 036 (54.1) | 282 881 (55.0) |
| Mean age (SD) | 51.0 (16.9) | 46.8 (16.0) | 50.0 (16.6) | 56.9 (16.5) |
| Weighted mean age (SD) | 47.8 (19.0) | 44.8 (16.8) | 46.8 (18.4) | 52.3 (22.2) |
| No. of current smokers (crude smoking rate) | 344 550 (21.6) | 139 537 (22.0) | 100 492 (22.6) | 104 521 (20.3) |
| No. of men smokers | 315 720 (43.6) | 127 334 (44.1) | 92 039 (45.0) | 96 347 (41.6) |
| No. of women smokers | 28 830 (3.3) | 12 203 (3.5) | 8453 (3.5) | 8174 (2.9) |
| Age-standardized smoking rate3 | 23.2 (23.1, 23.2) | 22.2 (22.1, 22.3) | 23.7 (23.6, 23.8) | 24.1 (23.9, 24.2) |
| Age-standardized smoking rate in men | 45.8 (45.6, 45.9) | 44.2 (44.0, 44.4) | 46.4 (46.2, 46.7) | 47.0 (46.7, 47.3) |
| Age-standardized smoking rate in women | 3.2 (3.1, 3.2) | 3.5 (3.4, 3.6) | 3.5 (3.4, 3.6) | 2.4 (2.3, 2.4) |
Source from the Community Health Survey in Korea, 2008-2014.
Values are presented as number (%) or % (95% confidence interval).
SD, standard deviation.
1 Metropolitan, urban and rural refers to “gu ”, “si ”, “gun ”, respectively.
2 The area deprivation index was calculated based on the 2010 Korean census data.
3 Age-standardized smoking rates were estimated with the 2010 Korean census population as the reference population, after taking into account the sample weights of the Community Health Survey.
- 1. Warren GW, Alberg AJ, Kraft AS, Cummings KM. The 2014 Surgeon General’s report: “The health consequences of smoking--50 years of progress”: a paradigm shift in cancer care. Cancer 2014;120(13):1914-1916ArticlePubMed
- 2. GBD 2013 Risk Factors Collaborators, Forouzanfar MH, Alexander L, Anderson HR, Bachman VF, Biryukov S, et al. Global, regional, and national comparative risk assessment of 79 behavioural, environmental and occupational, and metabolic risks or clusters of risks in 188 countries, 1990-2013: a systematic analysis for the Global Burden of Disease Study 2013. Lancet 2015;386(10010):2287-2323ArticlePubMedPMC
- 3. Choi S, Kim Y, Park S, Lee J, Oh K. Trends in cigarette smoking among adolescents and adults in South Korea. Epidemiol Health 2014;36: e2014023
- 4. Organization for Economic Cooperation and Development. Non-medical determinants of health. [cited 2016 Jun 21]. Available from: http://www.oecd-ilibrary.org/social-issuesmigration-health/data/oecd-health-statistics/oecd-healthdata-non-medical-determinants-of-health_data-00546-en
- 5. Khang YH, Cho HJ. Socioeconomic inequality in cigarette smoking: trends by gender, age, and socioeconomic position in South Korea, 1989-2003. Prev Med 2006;42(6):415-422ArticlePubMed
- 6. Park EJ, Kim H, Kawachi I, Kim IH, Cho SI. Area deprivation, individual socioeconomic position and smoking among women in South Korea. Tob Control 2010;19(5):383-390ArticlePubMed
- 7. Khang YH, Yun SC, Cho HJ, Jung-Choi K. The impact of governmental antismoking policy on socioeconomic disparities in cigarette smoking in South Korea. Nicotine Tob Res 2009;11(3):262-269ArticlePubMed
- 8. Khang YH, Lynch JW, Jung-Choi K, Cho HJ. Explaining age-specific inequalities in mortality from all causes, cardiovascular disease and ischaemic heart disease among South Korean male public servants: relative and absolute perspectives. Heart 2008;94(1):75-82ArticlePubMed
- 9. Ministry of Health and Welfare. Health Plan 2010. Seoul: Ministry of Health and Welfare; 2005. p. 211 (Korean)
- 10. Ministry for Health, Welfare and Family Affairs. Health Plan 2020. Seoul: Ministry for Health, Welfare and Family Affairs; 2011. p. 96 (Korean)
- 11. Ministry of Health and Welfare. Health Plan 2020. Sejong: Ministry of Health and Welfare; 2015. p. 36 (Korean)
- 12. Khang YH, Jung-Choi K, Cho SH, Cho HJ, Kim MH, Kim KW, et al. Health policy plan for tackling health inequalities in Seoul. Seoul: Seoul Metropolitan Goverment; 2012. p. 136-137 (Korean)
- 13. Jung-Choi K, Kong KA, Kim MH, Kim YM, Park JH, Yoon TH. Monitoring trends in health ineuqalities in Seoul. Seoul: Seoul Metropolitan Goverment; 2014. p. 67-77 (Korean)
- 14. Shin H, Lee S, Chu JM. Development of composite deprivation index for Korea: the correlation with standardized mortality ratio. J Prev Med Public Health 2009;42(6):392-402. (Korean)ArticlePubMedPDF
- 15. Choi MH, Cheong KS, Cho BM, Hwang IK, Kim CH, Kim MH, et al. Deprivation and mortality at the town level in Busan, Korea: an ecological study. J Prev Med Public Health 2011;44(6):242-248ArticlePubMedPMCPDF
- 16. Kim YT, Choi BY, Lee KO, Kim H, Chun JH, Kim SY, et al. Overview of Korean Community Health Survey. J Korean Med Assoc 2012;55(1):74-83. (Korean)Article
- 17. Khang YH, Kim HR. Socioeconomic mortality inequality in Korea: mortality follow-up of the 1998 National Health and Nutrition Examination Survey (NHANES) data. J Prev Med Public Health 2006;39(2):115-122. (Korean)PubMed
- 18. Bahk J, Khang YH. Trends in childhood obesity and central adiposity between 1998-2001 and 2010-2012 according to household income and urbanity in Korea. BMC Public Health 2016;16: 18ArticlePubMedPMCPDF
- 19. Korean Statistical Information Service. The household income and expenditure survey. Share by quintile and decile, household deficit ratio and boundaries (2 and more, household basis). [cited 2016 May 27]. Available from: http://kosis.kr/statHtml/statHtml.do?orgId=101&tblId=DT_1L6E004&vw_cd=MT_ZTITLE&list_id=G_A_4_3_1&seqNo=&lang_mode=ko&language=kor&obj_var_id=&itm_id=&conn_path=E1
- 20. Jarman B, Townsend P, Carstairs V. Deprivation indices. BMJ 1991;303(6801):523Article
- 21. Carstairs V. Deprivation indices: their interpretation and use in relation to health. J Epidemiol Community Health 1995;49 Suppl 2: S3-S8ArticlePubMed
- 22. Yoon TH, Noh M, Han J, Jung-Choi K, Khang YH. Deprivation and suicide mortality across 424 neighborhoods in Seoul, South Korea: a Bayesian spatial analysis. Int J Public Health 2015;60(8):969-976ArticlePubMed
- 23. Lopez AD, Collishaw NE, Piha T. A descriptive model of the cigarette epidemic in developed countries. Tob Control 1994;3(3):242-247ArticlePMC
- 24. Shortt NK, Tisch C, Pearce J, Mitchell R, Richardson EA, Hill S, et al. A cross-sectional analysis of the relationship between tobacco and alcohol outlet density and neighbourhood deprivation. BMC Public Health 2015;15: 1014ArticlePubMedPMCPDF
- 25. Pucci LG, Joseph HM Jr, Siegel M. Outdoor tobacco advertising in six Boston neighborhoods. Evaluating youth exposure. Am J Prev Med 1998;15(2):155-159ArticlePubMed
- 26. Barbeau EM, Wolin KY, Naumova EN, Balbach E. Tobacco advertising in communities: associations with race and class. Prev Med 2005;40(1):16-22ArticlePubMed
- 27. Ministry of Government Legislation. National Health Promotion Act: Article 9. 2014 [cited 2017 Feb 26]. Available from: http://www.law.go.kr/lsInfoP.do?lsiSeq=181391&efYd=2016#0000 (Korean)
- 28. Kim CS, Yun SC, Kim HR, Khang YH. A multilevel study on the relationship between the residential distribution of high class (power elites) and smoking in Seoul. J Prev Med Public Health 2006;39(1):30-38. (Korean)PubMed
- 29. Cho HJ, Khang YH, Yun SC. Occupational differentials in cigarette smoking in South Korea: findings from the 2003 Social Statistics Survey. J Prev Med Public Health 2006;39(4):365-370. (Korean)PubMed
- 30. Yeom KS. 2013 Convenience store. Seoul: Korean Association of Convenience Store Industry; 2013. p. 126-132 (Korean)
- 31. Kim MH, Seo JH, Son JI, Cho HJ, Choi YJ. Tobacco control policy in Korea and health inequalities. Seoul: People’s Health Institue; 2011. p. 140-143 (Korean)
- 32. Ling PM, Glantz SA. Why and how the tobacco industry sells cigarettes to young adults: evidence from industry documents. Am J Public Health 2002;92(6):908-916ArticlePubMedPMC
- 33. Sepe E, Ling PM, Glantz SA. Smooth moves: bar and nightclub tobacco promotions that target young adults. Am J Public Health 2002;92(3):414-419ArticlePubMedPMC
- 34. Scanlan JP. The mismeasure of health disparities. J Public Health Manag Pract 2016;22(4):415-419ArticlePubMed
- 35. Jung-Choi KH, Khang YH, Cho HJ. Hidden female smokers in Asia: a comparison of self-reported with cotinine-verified smoking prevalence rates in representative national data from an Asian population. Tob Control 2012;21(6):536-542ArticlePubMed
REFERENCES
Figure & Data
References
Citations

- Determinants of unhealthy living by gender, age group, and chronic health conditions across districts in South Korea using the 2010-2017 Community Health Surveys
Thi Tra Bui, Thi Huyen Trang Nguyen, Jinhee Lee, Sun Young Kim, Jin-Kyoung Oh
Epidemiology and Health.2024; : e2024014. CrossRef - Use of geographically weighted regression models to inform retail endgame strategies in South Korea: application to cigarette and ENDS prevalence
Heewon Kang, Eunsil Cheon, Jaeyoung Ha, Sung-il Cho
Tobacco Control.2023; : tc-2023-058117. CrossRef - Shift to a Younger Age and Regional Differences in Inflammatory Bowel Disease in Korea: Using Healthcare Administrative Data
Seo-Hee Kim, Yujin Park, Seong Pyo Kim, Sung Hee Lee, Seak Hee Oh, Suk-Kyun Yang, Hyung-Jin Yoon, Kyung Mo Kim
Digestive Diseases and Sciences.2022; 67(11): 5079. CrossRef - The Gaps in Health-Adjusted Life Years (HALE) by Income and Region in Korea: A National Representative Bigdata Analysis
Young-Eun Kim, Yoon-Sun Jung, Minsu Ock, Hyesook Park, Ki-Beom Kim, Dun-Sol Go, Seok-Jun Yoon
International Journal of Environmental Research and Public Health.2021; 18(7): 3473. CrossRef - Differential changes in quitting smoking by daily cigarette consumption and intention to quit after the introduction of a tobacco tax increase and pictorial cigarette pack warnings in Korea, 2013–2017
Ikhan Kim, Young-Ho Khang
Drug and Alcohol Dependence.2020; 213: 108085. CrossRef - Life Expectancy in Areas around Subway Stations in the Seoul Metropolitan Area in Korea, 2008–2017
Ikhan Kim, Hee-Yeon Kang, Young-Ho Khang
Journal of Korean Medical Science.2020;[Epub] CrossRef - Income differences in screening, incidence, postoperative complications, and mortality of thyroid cancer in South Korea: a national population-based time trend study
Hee-Yeon Kang, Ikhan Kim, Yeon-Yong Kim, Jinwook Bahk, Young-Ho Khang
BMC Cancer.2020;[Epub] CrossRef - A Multi-Disciplinary Study Into the Drivers of Smoking Cessation in South Korea
James E. Prieger, Anna Choi
SSRN Electronic Journal.2020;[Epub] CrossRef - Investigating the Drivers of Smoking Cessation: A Role of Alternative Nicotine Delivery Systems?
Sam Hampsher, James E. Prieger
SSRN Electronic Journal .2020;[Epub] CrossRef - Convenience store visitors recall cigarette advertisements even if they do not purchase cigarettes
Ji-eun Hwang, Sung-il Cho, Yu-seon Yang, Joung-eun Lee, Seon-young Lee, Yu-mi Oh
Journal of Public Health.2019; 41(4): 732. CrossRef - A spatial analysis of geographic variation and factors associated with hospitalization for bacterial pneumonia in Korea
Agnus M. Kim, Sungchan Kang, Jong Heon Park, Tae Ho Yoon, Yoon Kim
BMC Pulmonary Medicine.2019;[Epub] CrossRef - Hospitalizations for ambulatory care sensitive conditions as an indicator of access to primary care and excess of bed supply
Agnus M. Kim, Jong Heon Park, Tae Ho Yoon, Yoon Kim
BMC Health Services Research.2019;[Epub] CrossRef - An ecological study of geographic variation and factors associated with cesarean section rates in South Korea
Agnus M. Kim, Jong Heon Park, Sungchan Kang, Tae Ho Yoon, Yoon Kim
BMC Pregnancy and Childbirth.2019;[Epub] CrossRef - Long-term trends in smoking prevalence and its socioeconomic inequalities in Korea, 1992–2016
Youngs Chang, Hee-Yeon Kang, Dohee Lim, Hong-Jun Cho, Young-Ho Khang
International Journal for Equity in Health.2019;[Epub] CrossRef - A publicly well-accepted measure versus an academically desirable measure of health inequality: cross-sectional comparison of the difference between income quintiles with the slope index of inequality
Young-Ho Khang, Dohee Lim, Jinwook Bahk, Ikhan Kim, Hee-Yeon Kang, Youngs Chang, Kyunghee Jung-Choi
BMJ Open.2019; 9(6): e028687. CrossRef - Prevalence of Overweight and Income Gaps in 245 Districts of Korea: Comparison Using the National Health Screening Database and the Community Health Survey, 2009–2014
Ikhan Kim, Jinwook Bahk, Yeon-Yong Kim, Jeehye Lee, Hee-Yeon Kang, Juyeon Lee, Sung-Cheol Yun, Jong Heon Park, Soon-Ae Shin, Young-Ho Khang
Journal of Korean Medical Science.2018;[Epub] CrossRef - Comparison of District-level Smoking Prevalence and Their Income Gaps from Two National Databases: the National Health Screening Database and the Community Health Survey in Korea, 2009–2014
Ikhan Kim, Jinwook Bahk, Yeon-Yong Kim, Jeehye Lee, Hee-Yeon Kang, Juyeon Lee, Sung-Cheol Yun, Jong Heon Park, Soon-Ae Shin, Young-Ho Khang
Journal of Korean Medical Science.2018;[Epub] CrossRef - Clinical Significance of the Circle of Willis in Patients with Symptomatic Internal Carotid Artery Occlusion
Byoung Joo Park, Kang Min Kim, Woong Jae Lee, In Kook Chun, Inkyeong Kim, Seung Jin Lee, Seongheon Kim
World Neurosurgery.2018; 115: e585. CrossRef - Sensitivity analysis on the ecological bias for Seoul tuberculosis data
Eunjung Song, Soeun Kim, Seungsik Hwang, Woojoo Lee
Environmental and Ecological Statistics.2018; 25(3): 341. CrossRef - The Disease Burden of Lung Cancer Attributable to Residential Radon Exposure in Korean Homes
Jong-Hun Kim, Mina Ha
Journal of Korean Medical Science.2018;[Epub] CrossRef - Tobacco company strategies for maintaining cigarette
advertisements and displays in retail chain stores:
In-depth interviews with Korean convenience store owners
Ji-eun Hwang, Yu-mi Oh, Yu-seon Yang, Seon-young Lee, Joung-eun Lee, Sung-il Cho
Tobacco Induced Diseases.2018;[Epub] CrossRef - Income gaps in self-rated poor health and its association with life expectancy in 245 districts of Korea
Ikhan Kim, Jinwook Bahk, Sung-Cheol Yun, Young-Ho Khang
Epidemiology and Health.2017; 39: e2017011. CrossRef
 KSPM
KSPM

 PubReader
PubReader ePub Link
ePub Link Cite
Cite