Articles
- Page Path
- HOME > J Prev Med Public Health > Volume 53(4); 2020 > Article
-
COVID-19: Perspective
The Pandemic League of COVID-19: Korea Versus the United States, With Lessons for the Entire World -
Alwin Issac1
 , Shine Stephen1
, Shine Stephen1 , Jaison Jacob1
, Jaison Jacob1 , Vijay VR1
, Vijay VR1 , Rakesh Vadakkethil Radhakrishnan1
, Rakesh Vadakkethil Radhakrishnan1 , Nadiya Krishnan1
, Nadiya Krishnan1 , Manju Dhandapani2
, Manju Dhandapani2
-
Journal of Preventive Medicine and Public Health 2020;53(4):228-232.
DOI: https://doi.org/10.3961/jpmph.20.166
Published online: May 25, 2020
1College of Nursing, All India Institute of Medical Sciences (AIIMS), Bhubaneswar, India
2Post-Graduate Institute of Medical Education and Research (PGIMER), Chandigarh, India
- Corresponding author: Shine Stephen, MSN College of Nursing, All India Institute of Medical Sciences (AIIMS), Sijua, Post-Dumuduma, Patrapada, Bhubaneswar 751019, India E-mail: shinestephentn@gmail.com
Copyright © 2020 The Korean Society for Preventive Medicine
This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/by-nc/4.0/) which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
ABSTRACT
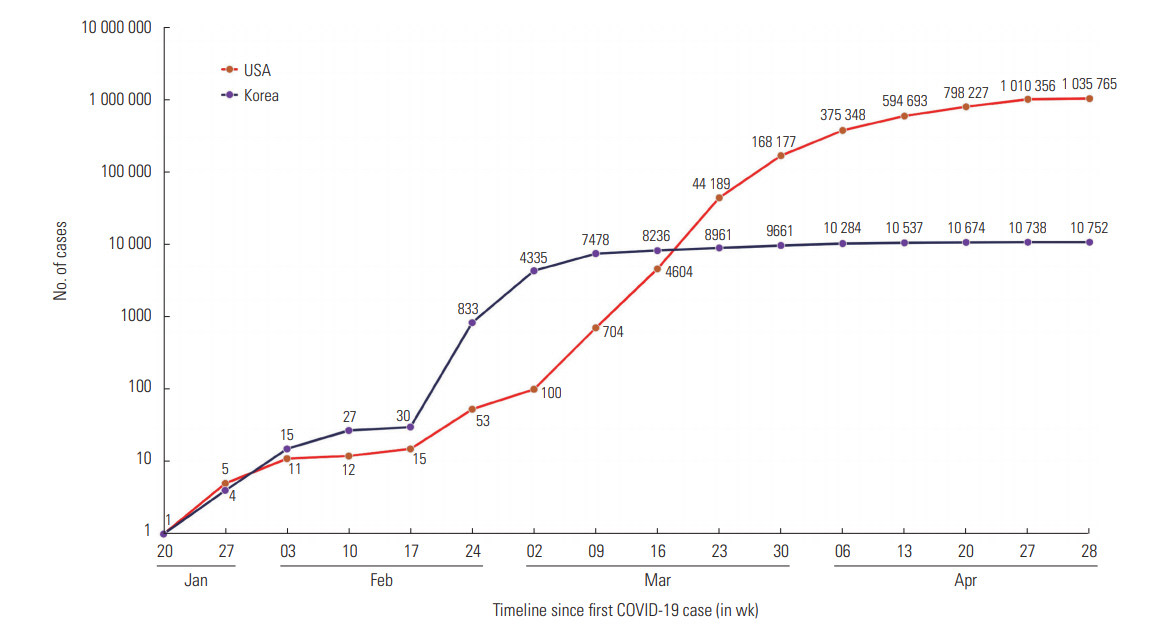
- Coronavirus disease 2019 (COVID-19) is inflicting a brutal blow on humankind, and no corner of the world has been exempted from its wrath. This study analyzes the chief control measures and the distinctive features of the responses implemented by Korea and the United States to contain COVID-19 with the goal of extracting lessons that can be applied globally. Even though both nations reported their index cases on the same day, Korea succeeded in flattening the curve, with 10 752 cases as of April 28, 2020, whereas the outbreak skyrocketed in the United States, which had more than 1 million cases at the same time. The prudent and timely execution of control strategies enabled Korea to tame the spread of the virus, whereas the United States paid a major price for its delay, although it is too early to render a conclusive verdict. Information pertaining to the number of people infected with the virus and measures instituted by the government to control the spread of COVID-19 was retrieved from the United States Centers for Disease Control and Prevention and the Korea Centers for Disease Control and Prevention websites and press releases. Drawing lessons from both nations, it is evident that the resolution to the COVID-19 pandemic lies in the prudent usage of available resources, proactive strategic planning, public participation, transparency in information sharing, abiding by the regulations that are put into place, and how well the plan of action is implemented.
- This paper is a perspective, so it did not need ethical approval.
Ethics Statement
-
CONFLICT OF INTEREST
The authors have no conflicts of interest associated with the material presented in this paper.
-
FUNDING
None.
Notes
ACKNOWLEDGEMENTS
-
AUTHOR CONTRIBUTIONS
Conceptualization: AI, SS. Data curation: JJ, RVR. Funding acquisition: None. Visualization: JJ. Writing – original draft: AI, SS, JJ, VVR, RVR. Writing – review & editing: NK, MD.
Notes

- 1. Worldometer. Coronavirus: COVID-19 coronavirus pandemic. [cited 2020 Apr 28]. Available from: https://www.worldometers.info/coronavirus/?fbclid=IwAR0RYMPhu-J9i5t74sla8KOrJFIhGMs--0YIuvQzoxLeFrvwwr5FLpn42Qw
- 2. World Bank. Population density (people per sq. km of land area) - Korea, Rep., United States. [cited 2020 Apr 29]. Available from: https://data.worldbank.org/indicator/EN.POP.DNST? locations=KR-US
- 3. United Nations Development Programme. Human development reports: 2019 Human Development Index ranking. [cited 2020 Apr 30]. Available from: http://hdr.undp.org/en/content/2019-human-development-index-ranking
- 4. Korea Centers for Disease Control & Prevention. The updates on COVID-19 in Korea as of 16 April. [cited 2020 May 20]. Available from: https://www.cdc.go.kr/board/board.es?mid=a30402000000&bid=0030&act=view&list_no=366909&tag=&nPage=1.%20Press%20release
- 5. COVID-19 National Emergency Response Center; Epidemiology & Case Management Team; Korea Centers for Disease Control & Prevention. Contact transmission of COVID-19 in South Korea: novel investigation techniques for tracing contacts. Osong Public Health Res Perspect 2020;11(1):60-63ArticlePubMedPMCPDF
- 6. Kwon KT, Ko JH, Shin H, Sung M, Kim JY. Drive-through screening center for COVID-19: a safe and efficient screening system against massive community outbreak. J Korean Med Sci 2020;35(11):e123ArticlePubMedPMC
- 7. Farrer M. Coronavirus: South Korea cluster drives huge rise in cases. The Guardian; 2020 Feb 22 [cited 2020 Apr 28]. Available from: https://www.theguardian.com/world/2020/feb/22/coronavirus-south-korea-sees-huge-jump-cases-china-hubei-wuhan-outbreak-
- 8. Wang J, Lindsay Huth L, Umlauf T. How the CDC’s restrictive testing guidelines hid the coronavirus epidemic: U.S. health officials’ slow response to the global spread led to a lag in testing. Wall Street Journal; 2020 Mar 22 [cited 2020 Apr 25]. Available from: https://www.wsj.com/articles/how-the-cdcs-restrictive-testing-guidelines-hid-the-coronavirus-epidemic-11584882001
- 9. Jernigan DB; CDC COVID-19 Response Team. Update: public health response to the coronavirus disease 2019 outbreak - United States, February 24, 2020. MMWR Morb Mortal Wkly Rep 2020;69(8):216-219ArticlePubMedPMC
- 10. Josh Margolin J, Meek JG. Intelligence report warned of coronavirus crisis as early as November: sources. ABC News; 2020 Apr 9 [cited 2020 Apr 23]. Available from: https://abcnews.go.com/Politics/intelligence-report-warned-coronavirus-crisis-early-novembr-sources/story?id=70031273
REFERENCES
Figure & Data
References
Citations

- Why do democracies respond differently to COVID-19? A comparison of the United States and South Korea
Yexin Mao
Frontiers in Public Health.2024;[Epub] CrossRef - Government Initiatives for Research Ethics During COVID-19 Pandemic in Korea
Young Su Park, Ock-Joo Kim
Journal of Korean Medical Science.2024;[Epub] CrossRef - CITIZENS’ PARTICIPATION IN INDONESIA’S COVID-19 PANDEMIC: A SYSTEMATIC LITERATURE REVIEW
Dewi Sekar Kencono, Achmad Djunaedi , Yuyun Purbokusumo
SSRN Electronic Journal.2024;[Epub] CrossRef - The role of veterinary diagnostic laboratories during COVID-19 response in the United States
Nia Clements, Diego G. Diel, François Elvinger, Gary Koretzky, Julie Siler, Lorin D. Warnick, Vittorio Sambri
PLOS ONE.2024; 19(6): e0303019. CrossRef - Assessing audit effort in response to exogenous shocks: Evidence from Korea on the impact of enhanced audit standards and COVID‐19
Jumi Kim, Meehyun Kim, Yangin Yoon, Won Gyun No, Miklos A. Vasarhelyi
International Journal of Auditing.2024;[Epub] CrossRef - An evidence-based nursing care guide for critically ill patients with COVID-19: A scoping Review
Manju Dhandapani, Vijay VR, Nadiya Krishnan, Lakshmanan Gopichandran, Alwin Issac, Shine Stephen, Jaison Jacob, Thilaka Thilaka, Lakshmi Narayana Yaddanapudi, Sivashanmugam Dhandapani
Asian Journal of Nursing Education and Research.2022; : 144. CrossRef - Assessing Knowledge, Preventive Practices, and Depression Among Chinese International Students and Local Korean Students in South Korea During the COVID-19 Pandemic: An Online Cross-Sectional Study
Xiaoxu Jiang, Bo Zhao, Eun Woo Nam, Fanlei Kong
Frontiers in Psychiatry.2022;[Epub] CrossRef - Enhancing the safety of frontline healthcare workers during coronavirus disease: a novel real-time remote audiovisual aided doffing approach
Manju Dhandapani, Sukhpal Kaur, Karobi Das, Rashmi Ranjan Guru, Manisha Biswal, Pranay Mahajan, Vipin Koushal, Goverdhan D. Puri
Infectious Diseases.2021; 53(2): 145. CrossRef - Beyond Doubt and Uncertainty: Religious Education for a Post-COVID-19 World
Hyun-Sook Kim
Religious Education.2021; 116(1): 41. CrossRef - The collateral fallout of COVID19 lockdown on patients with head injury from north-west India
Madhivanan Karthigeyan, Sivashanmugam Dhandapani, Pravin Salunke, Sushanta K. Sahoo, Mandeep S. Kataria, Apinderpreet Singh, Chandrashekhar Gendle, Chirag Panchal, Rajesh Chhabra, Kajal Jain, Sunil K. Gupta
Acta Neurochirurgica.2021; 163(4): 1053. CrossRef - Scrutiny of COVID-19 response strategies among severely affected European nations
Shine Stephen, Alwin Issac, Rakesh Vadakkethil Radhakrishnan, Jaison Jacob, VR Vijay, Sam Jose, SM Azhar, Anoop S. Nair, Nadiya Krishnan, Rakesh Sharma, Manju Dhandapani
Osong Public Health and Research Perspectives.2021; 12(4): 203. CrossRef - Generic Logic Model for Coronavirus Disease-2019 Responses Based on the South Korean Experience
Hae-ryoung Chun, Kyuhyun Yoon, Hana Kim, Eunsil Cheon, Jaeyoung Ha, Sangwoo Tak, Sung-il Cho
Risk Management and Healthcare Policy.2021; Volume 14: 4765. CrossRef - Effectiveness of public health measures in reducing the incidence of covid-19, SARS-CoV-2 transmission, and covid-19 mortality: systematic review and meta-analysis
Stella Talic, Shivangi Shah, Holly Wild, Danijela Gasevic, Ashika Maharaj, Zanfina Ademi, Xue Li, Wei Xu, Ines Mesa-Eguiagaray, Jasmin Rostron, Evropi Theodoratou, Xiaomeng Zhang, Ashmika Motee, Danny Liew, Dragan Ilic
BMJ.2021; : e068302. CrossRef - Social Distancing and Public Health Guidelines at Workplaces in Korea: Responses to Coronavirus Disease-19
Eun-A Kim
Safety and Health at Work.2020; 11(3): 275. CrossRef - COVID-19: Weighing the Endeavors of Nations, with Time to Event Analysis
Shine Stephen, Alwin Issac, Jaison Jacob, VR Vijay, Rakesh Vadakkethil Radhakrishnan, Nadiya Krishnan
Osong Public Health and Research Perspectives.2020; 11(4): 149. CrossRef - Challenges posed by COVID-19 and neurosurgical nursing strategies in developing countries
Manju Dhandapani, Sivashanmugam Dhandapani
Surgical Neurology International.2020; 11: 441. CrossRef - COVID-19: changing patterns among neurosurgical patients from North India, efficacy of repeat testing, and inpatient prevalence
Sushanta K. Sahoo, Sivashanmugam Dhandapani, Apinderpreet Singh, Chandrashekhar Gendle, Madhivanan Karthigeyan, Pravin Salunke, Ashish Aggarwal, Navneet Singla, Raghav Singla, Manjul Tripathi, Rajesh Chhabra, Sandeep Mohindra, Manoj Kumar Tewari, Manju Mo
Neurosurgical Focus.2020; 49(6): E7. CrossRef
 KSPM
KSPM

 PubReader
PubReader ePub Link
ePub Link Cite
Cite



