Articles
- Page Path
- HOME > J Prev Med Public Health > Volume 45(5); 2012 > Article
-
Correspondence
Author Response: The Increasing Hepatitis A Incidence in Korea: Is It Possible Within a Limited Time? - Joo Youn Seo1, Moran Ki2, Bo Youl Choi1
-
Journal of Preventive Medicine and Public Health 2012;45(5):331-332.
DOI: https://doi.org/10.3961/jpmph.2012.45.5.331
Published online: September 28, 2012
- 5,850 Views
- 70 Download
1Department of Preventive Medicine & Institute of Community Health, Hanyang University College of Medicine, Seoul, Korea.
2Department of Preventive Medicine, Eulji University School of Medicine, Daejeon, Korea.
- Corresponding author: Bo Youl Choi, MD, PhD. 222 Wangsimni-ro, Seongdong-gu, Seoul 133-791, Korea. Tel: +82-2-2220-0662, Fax: +82-2-2293-0660, bychoi@hanyang.ac.kr
Copyright © 2012 The Korean Society for Preventive Medicine
This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/by-nc/3.0/) which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
See the letter "Letter to the Editor: The Increasing Hepatitis A Incidence in Korea: Is It Possible Within a Limited Time?" on page 329.
- 1. Seo JY, Seo JH, Kim MH, Ki M, Park HS, Choi BY. Pattern of hepatitis a incidence according to area characteristics using national health insurance data. J Prev Med Public Health 2012;45(3):164-173. 22712043ArticlePubMedPMCPDF
- 2. Health Insurance Review and Assessment Service. National Health Insurance Corporation. 2009 National health insurance statistical yearbook. 2010. Seoul: Health Insurance Review and Assessment Service, National Health Insurance Corporation; p. 5-6 (Korean)
- 3. Ki M, Park T, Yi SG, Oh JK, Choi B. Risk analysis of aseptic meningitis after measles-mumps-rubella vaccination in Korean children by using a case-crossover design. Am J Epidemiol 2003;157(2):158-165. 12522023ArticlePubMed
- 4. Choi HJ, Lee SY, Ma SH, Kim JH, Hur JK, Kang JH. Age related prevalence of antibodies to hepatitis A virus, performed in Korea in 2005. Korean J Pediatr Infect Dis 2005;12(2):186-194. (Korean)ArticlePDF
- 5. Kim JH. Recent epidemiological status and vaccination of hepatitis A in Korea. J Korean Med Assoc 2008;51(2):110-118. (Korean)Article
REFERENCES
Figure 2The 2008 nationwide of Korea hepatitis A incidence (/100 000) according to deprivation index and population density of area. From Seo et al. Pattern of hepatitis a incidence according to area characteristics using national health insurance data. J Prev Med Public Health 2012;45(3):164-173 [1].
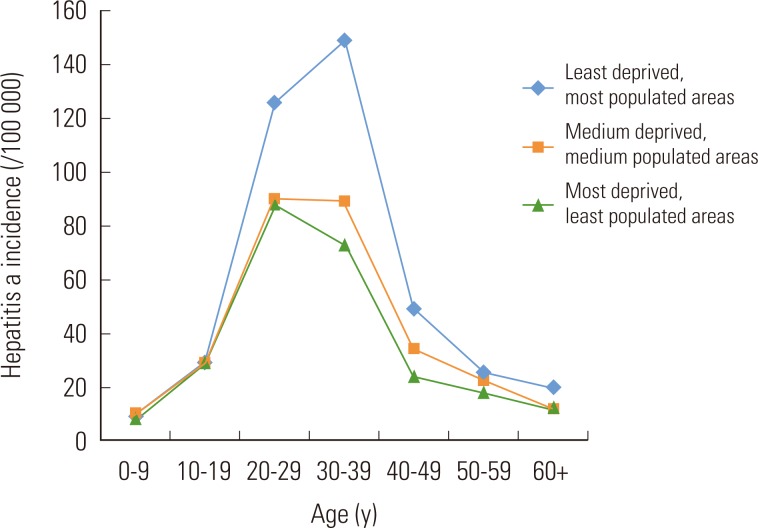

Figure & Data
References
Citations
Citations to this article as recorded by 

 KSPM
KSPM


 PubReader
PubReader ePub Link
ePub Link Cite
Cite



