Articles
- Page Path
- HOME > J Prev Med Public Health > Volume 56(1); 2023 > Article
-
Original Article
The Effect of Cognitive Impairment on the Association Between Social Network Properties and Mortality Among Older Korean Adults -
Eunji Kim1
 , Kiho Sung2
, Kiho Sung2 , Chang Oh Kim3
, Chang Oh Kim3 , Yoosik Youm2
, Yoosik Youm2 , Hyeon Chang Kim1,4
, Hyeon Chang Kim1,4
-
Journal of Preventive Medicine and Public Health 2023;56(1):31-40.
DOI: https://doi.org/10.3961/jpmph.22.350
Published online: November 22, 2022
- 4,391 Views
- 164 Download
1Department of Preventive Medicine, Yonsei University College of Medicine, Seoul, Korea
2Department of Sociology, Yonsei University Graduate School, Seoul, Korea
3Division of Geriatrics, Department of Internal Medicine, Yonsei University College of Medicine, Seoul, Korea
4Department of Public Health, Yonsei University Graduate School, Seoul, Korea
- Corresponding author: Hyeon Chang Kim, Department of Preventive Medicine, Yonsei University College of Medicine, 50-1 Yonsei-ro, Seodaemun-gu, Seoul 03722, Korea E-mail: hckim@yuhs.ac
- Co-corresponding author: Yoosik Youm, Department of Sociology, Yonsei University Graduate School, 50 Yonsei-ro, Seodaemun-gu, Seoul 03722, Korea E-mail: yoosik@yonsei.ac.kr
Copyright © 2023 The Korean Society for Preventive Medicine
This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/by-nc/4.0/) which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
ABSTRACT
-
Objectives:
- This study investigated the effect of cognitive impairment on the association between social network properties and mortality among older Korean adults.
-
Methods:
- This study used data from the Korean Social Life, Health, and Aging Project. It obtained 814 older adults’ complete network maps across an entire village in 2011-2012. Participants’ deaths until December 31, 2020 were confirmed by cause-of-death statistics. A Cox proportional hazards model was used to assess the risks of poor social network properties (low degree centrality, perceived loneliness, social non-participation, group-level segregation, and lack of support) on mortality according to cognitive impairment.
-
Results:
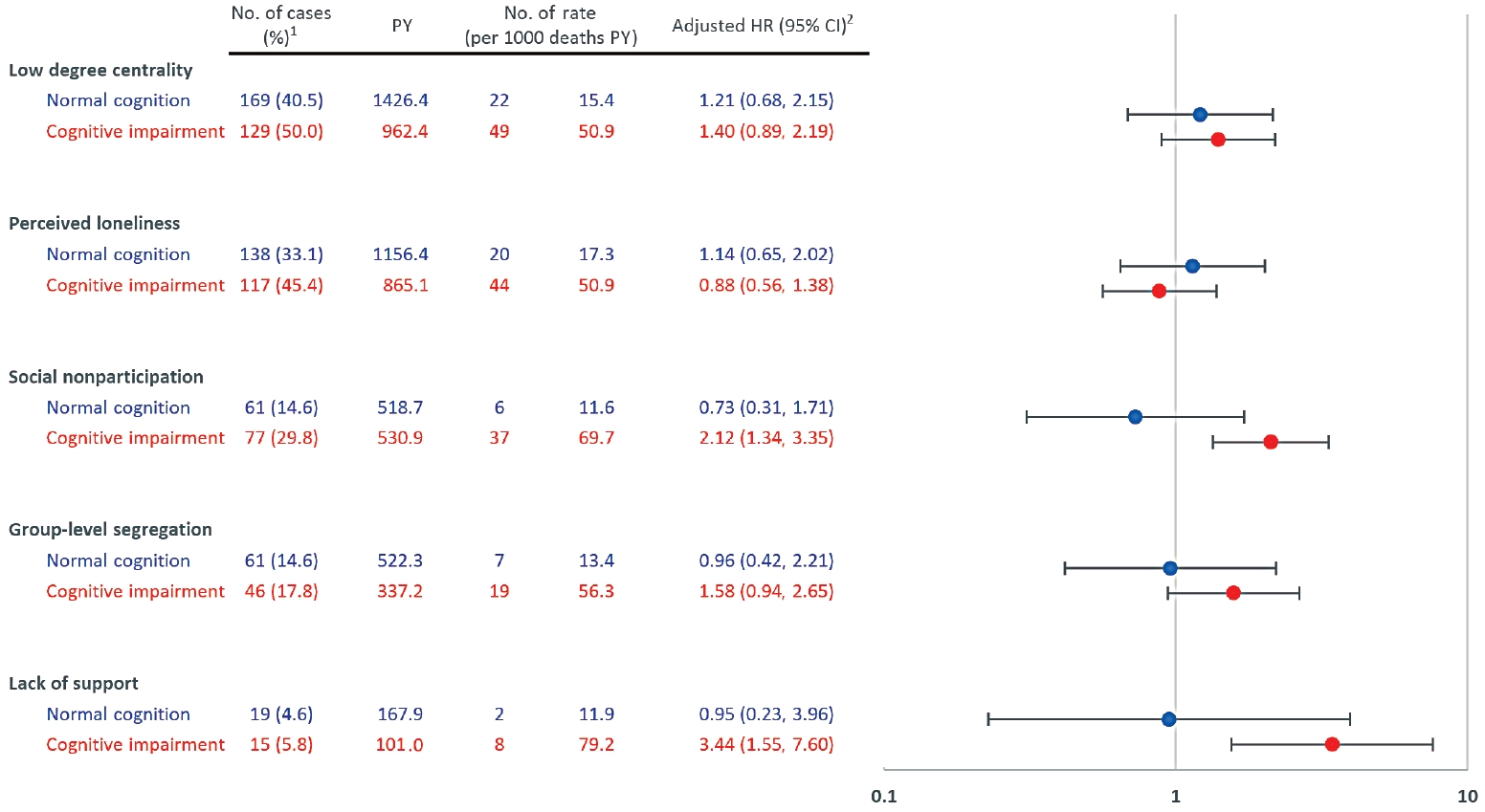
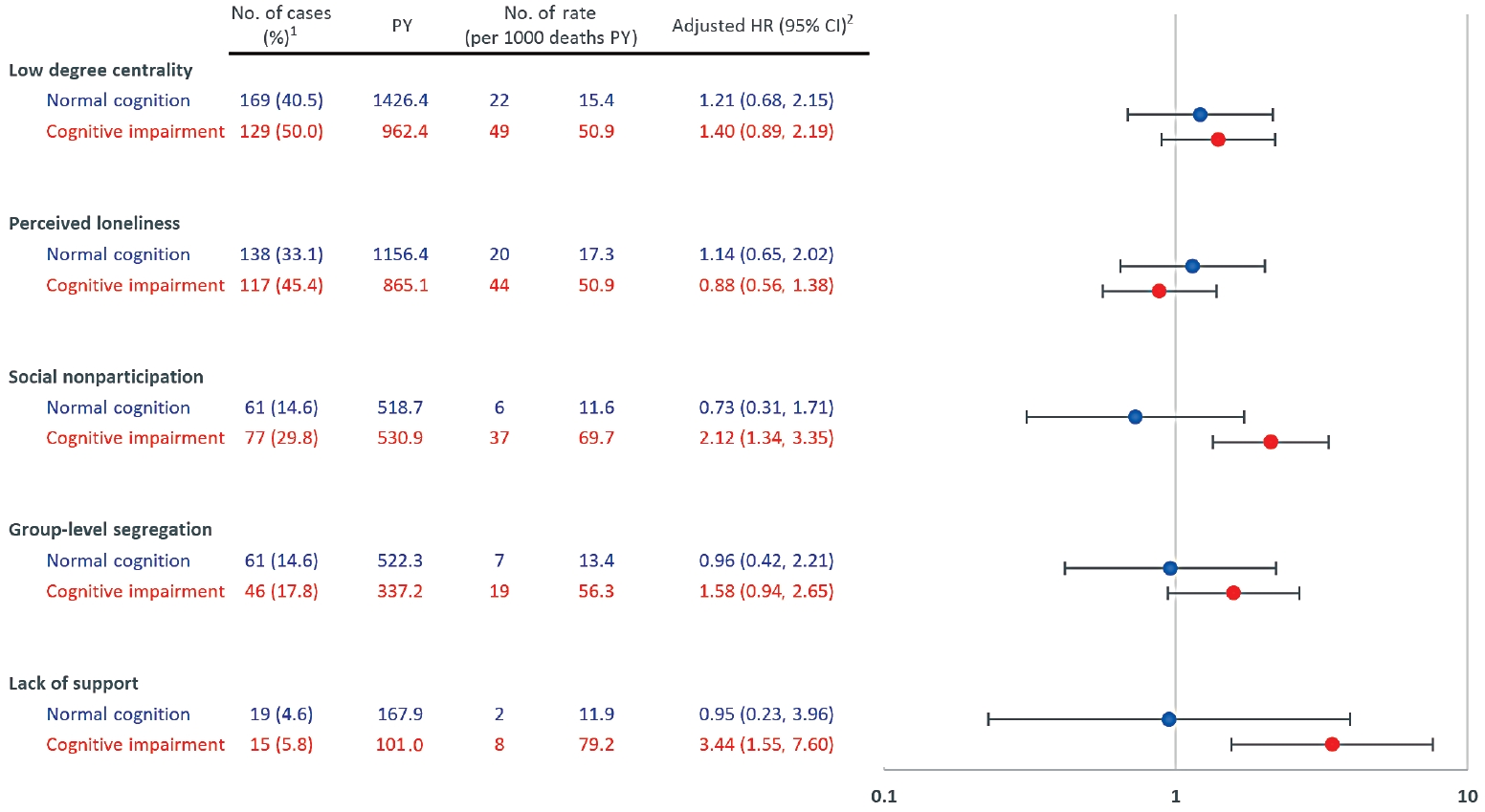
- In total, 675 participants (5510.4 person-years) were analyzed, excluding those with missing data and those whose deaths could not be verified. Along with cognitive impairment, all social network properties except loneliness were independently associated with mortality. When stratified by cognitive function, some variables indicating poor social relations had higher risks among older adults with cognitive impairment, with adjusted hazard ratios (HRs) of 2.12 (95% confidence interval [CI], 1.34 to 3.35) for social non-participation, 1.58 (95% CI, 0.94 to 2.65) for group-level segregation, and 3.44 (95% CI, 1.55 to 7.60) for lack of support. On the contrary, these effects were not observed among those with normal cognition, with adjusted HRs of 0.73 (95% CI, 0.31 to 1.71), 0.96 (95% CI, 0.42 to 2.21), and 0.95 (95% CI, 0.23 to 3.96), respectively.
-
Conclusions:
- The effect of social network properties was more critical among the elderly with cognitive impairment. Older adults with poor cognitive function are particularly encouraged to participate in social activities to reduce the risk of mortality.
- An extensive body of literature indicates that the quantity and quality of social networks have decreased in recent years [1]. Prevalent loneliness and social isolation in industrialized societies have caused public health problems [2]. For instance, the cumulative effect of loneliness has been found to be associated with the number of risk factors for cardiovascular diseases, such as elevated body mass index, systolic blood pressure, and total cholesterol levels, as well as low levels of high-density lipoprotein cholesterol [3]. Moreover, many studies have illustrated the impact of social relationships on mortality. Despite various definitions of social network properties and study populations, a poor social network has been consistently observed to be a strong predictor of mortality [4]. A meta-analysis including 148 studies demonstrated a 50% higher likelihood of mortality among those without sufficient social relations compared to those with sufficient social relations [5]. These effects of social network properties on mortality are comparable to the well-known risk factors of premature death, such as smoking, obesity, and physical inactivity [5].
- Poor cognitive function has also shown associations with an increased risk of mortality in several studies [6]. Cognitive impairment, as measured by the Mini-Mental State Examination (MMSE) score, increases the risk of all-cause and cardiovascular disease mortality [6,7]. Cognitive impairment does not necessarily refer to only dementia, and encompasses mild cognitive decline. Literature on older adults with cognitive impairment, but without dementia, has repeatedly reported higher risks of progressing to dementia and premature death [8].
- Although the associations of mortality with specific social aspects or cognitive function have been considerably studied, their combined effect remains unclear. Thus, this study aimed to investigate the effect of cognitive impairment on the association between social network properties and mortality among older Korean adults in a rural community.
INTRODUCTION
- Study Participants
- This study was conducted using data from the Korean Social Life, Health and Aging Project (KSHAP) study, which examined the entire population aged 60 or older in Village K, a typical rural community in Ganghwa, Korea, and collected complete social network maps for the elderly inhabitants of the village [9,10]. Among the target population (860 residents), 814 older adults and their spouses participated in the baseline survey from December 2011 to March 2012 (a response rate of 94.65%). Among them, 697 participants enrolled with personal identification numbers that make it possible to link to cause-of-death statistics. Those with missing data for social network properties, age, sex, education level, smoking, drinking, or comorbidities were excluded. In total, 675 respondents (5510.4 person-years) were analyzed in this study (Supplemental Material 1).
- Measures
- Using the complete network maps of the whole village, degree centrality was calculated as the number of social relations that a respondent had. Our analyses employed all-degree centrality, which includes both in-degree and out-degree centrality (i.e., the number of people who identify a participant as a network member and vice versa, respectively) [9]. We categorized participants as having higher or lower centrality compared to the median value of 4.0. Perceived loneliness was defined as feeling lonely for more than 1 day or 2 days over the past week based on the Center for Epidemiologic Studies Depression Scale questionnaires. Social non-participation was defined as not participating in any of the following 7 social activities: senior citizens’ associations, volunteering, religious activities, meetings for friendship, hobbies, local associations, or senior job placement projects. The complete social network also made it possible to identify groups (components) where each respondent was connected within and separated by other groups. There were two types of components: strong and weak components. In strong components, every person was reachable by others following the directions of the discussion network, but not necessarily following the directions in weak components [11]. The KSHAP study identified 537 strong and 85 weak components [9]. As Village K is a typical rural community where relations between residents are relatively close and strong, weak components were used for our analyses to understand the effect of social dynamics. Among the weak components, ranging from 1 person to 757 persons, group-level segregation referred to belonging to a social group with a relatively limited range (66 persons or less in a component). Lack of support was defined as participants responding that they could not rely on any of their spouses, family members, relatives, friends, or neighbors when having a problem.
- The Korean version of the Mini-Mental State Examination for Dementia Screening (K-MMSE) was used for the evaluation of cognitive function in the KSHAP study [10]. The K-MMSE has been established as a reliable and valid tool for screening cognitive impairment or dementia in a community setting [12]. The score ranges from 0 to 30. Based on previous studies, we categorized those with a score of 23 or less as having cognitive impairment and those with a score of 24 or more as having normal cognition [13-15].
- Among participants, deaths until December 31, 2020 were confirmed using cause-of-death statistics. The observed period was from the first survey date to the death date on the basis of death certificates for event cases or to the last day of observation (December 31, 2020) for censored cases in this study.
- Socio-demographic characteristics included age, sex, and educational attainment. The educational attainment level was categorized as no formal education, middle school or less, and high school or above. The health-related covariates included smoking status, alcohol use, and comorbidities. Among the diseases studied in the KSHAP study, hypertension, diabetes, cancer, stroke, and coronary heart disease were considered in our analyses, as the previous literature demonstrated that they increase mortality in the older population [16,17].
- Statistical Analysis
- Along with the total study population, socio-demographic characteristics and social network properties were compared between those with normal cognition and with cognitive impairment using the t-test and chi-square test. Using a Cox proportional hazards model, the associations of low degree centrality, perceived loneliness, social non-participation, group-level segregation, and lack of support with the risk of all-cause death were evaluated. Kaplan-Meier curves were plotted according to social network properties and cognitive function. The proportional hazards assumption was also assessed for each variable using weighted Schoenfeld residuals. Unadjusted and adjusted hazard ratios (HRs) were presented with 95% confidence intervals (CIs). The multivariate model was adjusted for age, sex, educational attainment, smoking, drinking, and comorbidity. Identical analyses were repeated after stratifying by cognitive function. All analyses were carried out using SAS version 9.4 (SAS Institute Inc., Cary, NC, USA).
- Ethics Statement
- The KSHAP study was conducted with approval from the Institutional Review Board of Yonsei University (YUIRB-2011–012-01) in 2011. The current study was approved by the Yonsei University Health System, Severance Hospital (4-2021-1401) in 2021.
METHODS
Social network properties
Cognitive impairment
Mortality
Covariates
- The socio-demographic characteristics and social network properties of the study population stratified by cognitive function are described in Table 1. The group with cognitive impairment had a higher proportion of older, female, and less-educated participants. They were also likely to show poor characteristics for all social network properties studied, although the prevalence of group-level segregation and lack of support was not statistically significantly different compared to those with normal cognition. The distributions of K-MMSE scores are also presented in Supplemental Material 2. The mean values of the scores were 23.94 among all participants, 26.79 among those with normal cognition, and 19.34 among those with cognitive impairment.
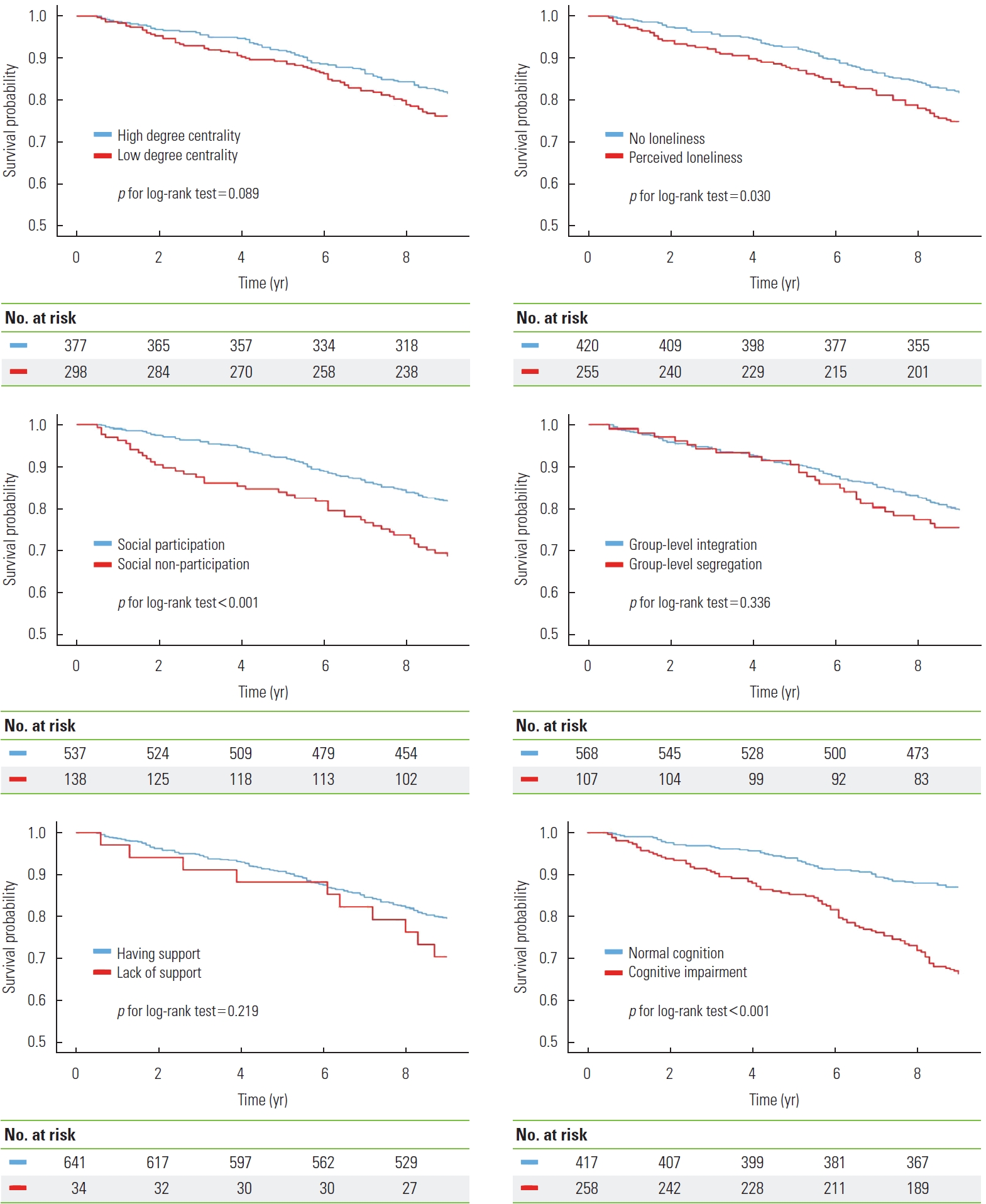
- In Figure 1, the Kaplan-Meier curves and risk tables were plotted according to each characteristic of social networks and cognitive function. Older adults with low degree centrality, loneliness, social non-participation, group-level segregation, and cognitive impairment had a lower survival rate than each corresponding group. Additively, independence between the Schoenfeld residuals for each variable and time was diagnosed, and the proportional hazards assumption was confirmed (Supplemental Material 3).
- Table 2 shows the results of the unadjusted and adjusted Cox proportional hazards regression between social network properties or cognitive function and mortality. After adjusting for covariates, participants with cognitive impairment had a higher risk of mortality (adjusted hazard ratio [aHR], 1.71; 95% CI, 1.15 to 2.54) than those with normal cognition. In terms of social network properties, participants with all types of insufficient networks except perceived loneliness (aHR, 1.04; 95% CI, 0.74 to 1.47) showed significantly higher aHRs than their counterparts, although only the associations for social non-participation and lack of support were statistically significant (aHR, 1.64; 95% CI, 1.12 to 2.39 for social non-participation and aHR, 2.13; 95% CI, 1.10 to 4.13 for lack of support).
- Figure 2 depicts different effects of social network properties on mortality according to cognitive function. Low degree centrality and perceived loneliness had similar HRs for mortality regardless of cognitive function. However, social non-participation significantly increased the risk of mortality among the elderly with cognitive impairment (aHR, 2.12; 95% CI, 1.34 to 3.35), whereas the effect of social non-participation was not observed among those with normal cognition. Likewise, group-level segregation among those with cognitive impairment showed an aHR of 1.58 (95% CI, 0.94 to 2.65) and lack of support had an aHR of 3.44 (95% CI, 1.55 to 7.60). In an additional analysis of the interaction between social network properties and cognitive function on mortality, only social non-participation showed statistical significance (Supplemental Material 4).
RESULTS
- This study investigated the effect of cognitive impairment on the association between social network properties and mortality using data from the KSHAP study from 2011 to 2020. Overall, our result is consistent with previous studies showing that individuals with weak social networks had a lower likelihood of survival than those with sufficient networks [5]. Additionally, older adults with cognitive impairment showed a higher prevalence of having fewer social ties, feeling lonely, and not participating in any activities. Furthermore, these social network properties had a greater influence on mortality among older persons with cognitive impairment, compared to those with normal cognition.
- Our study classified the magnitude of social relations using the median value of 4.0 in degree centrality, and showed increased mortality in people with low centrality than in people with high centrality. Several studies have reported that social network size is strongly associated with mortality, although it is unclear which number of social connections is most influential [18]. One study in the United States showed that social interactions with 0-1 friend had an HR of 1.32 for mortality compared to those with 6-7 friends [18]. However, another study implied different effects between strong and weak ties on mortality; the risk of premature death was not necessarily increased with a small number of strong ties, but did show such a relationship with a small number of weak ties [19]. To investigate the optimal size of a social network, further research is required with consideration of the characteristics of social networks besides the number of connections.
- Social non-participation significantly increased the risk of premature death in our study (aHR, 1.64; 95% CI, 1.12 to 2.39). Considering that the KSHAP study examined relatively healthy participants at baseline in a community-based setting and adjusted for other covariates, social non-participation per se, at least, partly accounts for a loss of physical health. A study in Japan, which is challenged by an aging society, showed that social participation increased the probability of survival in older people [20]. Social activities—in particular, those relating to personal development, such as educational and physical activities, and short-term employment—resulted in lower hazards of death [20]. Participating in social activities may lead to the attainment of health information and access to health care services as well as its psychosocial benefits [21,22].
- Lack of support was the strongest predictor of premature death in this study. The unadjusted HR was 1.49 (95% CI, 0.78 to 2.84), and the fully aHR was 2.13 (95% CI, 1.10 to 4.13). When independently controlling for each covariate, the increased strength of the association was mainly due to adjustment for age (Supplemental Material 5). Age seemed to weaken the association between lack of support and mortality in our study, where the participants with support tend to be older than those without (Supplemental Material 6). Older age increases mortality, but it is not known whether older age is associated with a higher likelihood of lack of support. Further studies need to reaffirm the association between age and lack of support with a larger sample. The protective effect of having support has been illustrated in previous research. Being embedded in a social network has a protective effect by giving individuals meaningful roles, generating self-esteem, and providing a sense of purpose in life [23]. Moreover, when stratified, the absence of timely help from a partner, family, and friends was more critical among the elderly who experienced a physical and cognitive decline (aHR, 3.44; 95% CI, 1.55 to 7.60). This may reflect, for instance, increased difficulties in the utilization of healthcare services and reduced motivation for healthier behaviors [24].
- The complete-network analyses in the KSHAP study showed that insufficient social network properties at a group level also increased the risk of mortality. Social isolation at the group level, as well as at the individual level, was associated with a higher risk of mortality [17]. Participants classified as having group-level segregation may have been not isolated individually and may have even had strong and frequent social connections with others in the same group. Nevertheless, belonging to a group with a small diameter was associated with an increased risk of premature death. Group-level segregation may confine older adults to limited health information and hinder them from accessing a broad range of health services [25,26].
- Along with social network properties, cognitive impairment had a significant influence on mortality. Univariate analysis showed an HR of 2.91 (95% CI, 2.07 to 4.08) for cognitive impairment, and the higher risk was persistent after adjusting for covariates. This finding is consistent with other studies; one prospective study suggested that cognitive impairment was the strongest predictor of mortality, in particular deaths from ischemic stroke [6,27]. When considering both social network properties and cognitive function, the effect of social network properties on mortality differed by cognitive function. Social non-participation, group-level segregation, and lack of support increased the risk of mortality only among older adults with cognitive impairment, while the increased risk associated with social network size did not show a difference between those with normal cognition and without. To our knowledge, there is little research on the effect of cognitive function on the association between social network properties and mortality. One study using the National Health and Nutrition Examination Survey in the United States illustrated that cognitive impairment and social network properties each raised the risk of premature death, but did not observe the interaction between them [28]. Although further studies are required to fully explain the different effects of social network properties on mortality by cognitive function, there are some possible explanations; for instance, the protective effect of sufficient social network properties appears to be more critical among older adults with cognitive impairment than those without. For instance, emotional and psychosocial benefits, such as the stress-buffering effect from social interactions, could be stronger in older adults with cognitive decline [29]. Cognitive function may also influence the degree to which people obtain health information, access health care services, and facilitate positive health behaviors that are obtained through sufficient social relationships [4,30]. Cognitive function is related to the associations between health literacy and physical health among older adults, and it has been known as a significant risk factor for premature death [30].
- Our study has some strengths in its investigation of the effect of cognitive impairment on the association between social network properties and mortality among older Korean adults. The KSHAP data enabled us to analyze various types of social relations. The complete social network analyses of all participants in the village provided both individual-level and group-level characteristics of the social network. Since the study population showed a high response rate (94.65%) and was relatively homogeneous in educational achievement and occupation, the study findings are unlikely to be severely confounded by socioeconomic status. Although the implications of this study could be relevant for epidemiological studies and community health settings, several limitations should also be taken into consideration. First, the results may not be generalizable to other populations, since they were derived from a study of older adults in a rural village in Korea. Second, the small sample size might undermine the findings. Further studies with larger sample sizes and longer follow-up periods are required to reaffirm the varying effects of cognitive impairment on the association between social network properties and mortality. Third, we defined cognitive impairment using the K-MMSE score rather than clinical diagnoses. Although there are some arguments regarding the use of the MMSE to screen for cognitive impairment, it is a valid and reliable tool, particularly in a community-based setting [12,15]. A considerable body of research suggests a general cut-point of 23/24 for the MMSE could be appropriate for detecting mild cognitive impairment and dementia in the general population [31,32]. Fourth, response bias, such as social-desirability bias, might have influenced our results. In terms of social network properties, survey participants could respond in a manner that would be viewed favorably by others (e.g., overrating their social network properties) [33]. Fifth, we adjusted for 5 comorbidities known to increase mortality in older adults: hypertension, diabetes, cancer, stroke, and coronary heart disease. Although previous studies have also suggested that social network properties per se are associated with an increased risk of morbidity and mortality, regardless of underlying diseases, the possibility should be taken into account that other diseases not included could affect our results [4]. Last, there was a possibility of residual confounding, as time-varying confounding variables were not sufficiently controlled, although we evaluated the proportional hazards assumption by confirming independence between the Schoenfeld residuals and time.
- According to our study, it is crucial for older adults to have sufficient and strong social networks. Furthermore, the effects of social network properties were more critical among older adults with cognitive impairment, who are particularly encouraged to participate in social activities and be integrated into social networks to reduce the risk of mortality.
DISCUSSION
SUPPLEMENTAL MATERIALS
Supplemental Material 1.
Supplemental Material 2.
Supplemental Material 3.
Supplemental Material 4.
Supplemental Material 5.
Supplemental Material 6.
-
CONFLICT OF INTEREST
The authors have no conflicts of interest associated with the material presented in this paper.
-
FUNDING
This work used data from the KSHAP study, which was supported by the Ministry of Education of the Republic of Korea, the National Research Foundation of Korea (grant No. NRF-2017S1A3A2067165).
-
AUTHOR CONTRIBUTIONS
Conceptualization: Kim E, Kim HC. Data curation: Youm Y, Kim HC, Kim CO, Sung K. Formal analysis: Kim E. Funding acquisition: Youm Y. Methodology: Kim E, Kim HC, Youm Y. Visualization: Kim E. Writing – original draft: Kim E, Sung K. Writing – review & editing: Kim CO, Youm Y, Kim HC.
Notes
ACKNOWLEDGEMENTS
| Variables | No. of deaths | PY | Rate (per 1000 PY) |
HR (95% CI) |
|
|---|---|---|---|---|---|
| Unadjusted | Adjusted1 | ||||
| Low degree centrality | |||||
| No | 70 | 3121.6 | 22.4 | 1.00 (reference) | 1.00 (reference) |
| Yes | 71 | 2388.8 | 29.7 | 1.33 (0.96, 1.85) | 1.35 (0.95, 1.91) |
| Perceived loneliness | |||||
| No | 77 | 3488.9 | 22.1 | 1.00 (reference) | 1.00 (reference) |
| Yes | 64 | 2021.5 | 31.7 | 1.44 (1.04, 2.01) | 1.04 (0.74, 1.47) |
| Social non-participation | |||||
| No | 98 | 4460.8 | 22.0 | 1.00 (reference) | 1.00 (reference) |
| Yes | 43 | 1049.6 | 41.0 | 1.88 (1.31, 2.69) | 1.64 (1.12, 2.39) |
| Group-level segregation | |||||
| No | 115 | 4650.9 | 24.7 | 1.00 (reference) | 1.00 (reference) |
| Yes | 26 | 859.5 | 30.3 | 1.23 (0.81, 1.89) | 1.37 (0.89, 2.10) |
| Lack of support | |||||
| No | 131 | 5241.5 | 25.0 | 1.00 (reference) | 1.00 (reference) |
| Yes | 10 | 268.9 | 37.2 | 1.49 (0.78, 2.84) | 2.13 (1.10, 4.13) |
| Cognitive impairment | |||||
| No | 54 | 3525.2 | 15.3 | 1.00 (reference) | 1.00 (reference) |
| Yes | 87 | 1985.2 | 43.8 | 2.91 (2.07, 4.08) | 1.71 (1.15, 2.54) |
- 1. Luo Y, Hawkley LC, Waite LJ, Cacioppo JT. Loneliness, health, and mortality in old age: a national longitudinal study. Soc Sci Med 2012;74(6):907-914ArticlePubMedPMC
- 2. Hawkley LC, Cacioppo JT. Loneliness matters: a theoretical and empirical review of consequences and mechanisms. Ann Behav Med 2010;40(2):218-227ArticlePubMed
- 3. Caspi A, Harrington H, Moffitt TE, Milne BJ, Poulton R. Socially isolated children 20 years later: risk of cardiovascular disease. Arch Pediatr Adolesc Med 2006;160(8):805-811ArticlePubMed
- 4. Holt-Lunstad J, Smith TB. Social relationships and mortality. Soc Personal Psychol Compass 2012;6(1):41-53ArticlePDF
- 5. Holt-Lunstad J, Smith TB, Layton JB. Social relationships and mortality risk: a meta-analytic review. PLoS Med 2010;7(7):e1000316ArticlePubMedPMC
- 6. Gale CR, Martyn CN, Cooper C. Cognitive impairment and mortality in a cohort of elderly people. BMJ 1996;312(7031):608-611ArticlePubMedPMC
- 7. An J, Li H, Tang Z, Zheng D, Guo J, Liu Y, et al. Cognitive impairment and risk of all-cause and cardiovascular disease mortality over 20-year follow-up: results from the BLSA. J Am Heart Assoc 2018;7(15):e008252ArticlePubMedPMC
- 8. Palmer K, Fratiglioni L, Winblad B. What is mild cognitive impairment? Variations in definitions and evolution of nondemented persons with cognitive impairment. Acta Neurol Scand Suppl 2003;179: 14-20ArticlePubMedPDF
- 9. Youm Y, Laumann EO, Ferraro KF, Waite LJ, Kim HC, Park YR, et al. Social network properties and self-rated health in later life: comparisons from the Korean social life, health, and aging project and the national social life, health and aging project. BMC Geriatr 2014;14: 102ArticlePubMedPMCPDF
- 10. Lee JM, Lee WJ, Kim HC, Choi W, Lee J, Sung K, et al. The Korean social life, health and aging project-health examination cohort. Epidemiol Health 2014;36: e2014003ArticlePubMedPMC
- 11. Scott J. Social network analysis. 3rd ed. Los Angeles: SAGE; 2013. p. 117-119
- 12. Jeong SK, Cho KH, Kim JM. The usefulness of the Korean version of modified Mini-Mental State Examination (K-mMMSE) for dementia screening in community dwelling elderly people. BMC Public Health 2004;4: 31ArticlePubMedPMCPDF
- 13. Kim S, Kim Y, Park SM. Association between alcohol drinking behaviour and cognitive function: results from a nationwide longitudinal study of South Korea. BMJ Open 2016;6(4):e010494ArticlePubMedPMC
- 14. Choi YJ, Hong YC, Do YK. The effects of social activities and living arrangements on cognitive functions in middle-aged and elderly adults: a panel study using the 2006-2018 Korean Longitudinal Study of Aging. J Prev Med Public Health 2021;54(6):395-403ArticlePubMedPMCPDF
- 15. Tombaugh TN, McIntyre NJ. The mini-mental state examination: a comprehensive review. J Am Geriatr Soc 1992;40(9):922-935ArticlePubMed
- 16. Fillenbaum GG, Pieper CF, Cohen HJ, Cornoni-Huntley JC, Guralnik JM. Comorbidity of five chronic health conditions in elderly community residents: determinants and impact on mortality. J Gerontol A Biol Sci Med Sci 2000;55(2):M84-M89ArticlePubMed
- 17. Youm Y, Baldina E, Baek J. All-cause mortality and three aspects of social relationships: an eight-year follow-up of older adults from one entire Korean village. Sci Rep 2021;11(1):465ArticlePubMedPMCPDF
- 18. Becofsky KM, Shook RP, Sui X, Wilcox S, Lavie CJ, Blair SN. Influence of the source of social support and size of social network on all-cause mortality. Mayo Clin Proc 2015;90(7):895-902ArticlePubMed
- 19. Kauppi M, Kawachi I, Batty GD, Oksanen T, Elovainio M, Pentti J, et al. Characteristics of social networks and mortality risk: evidence from 2 prospective cohort studies. Am J Epidemiol 2018;187(4):746-753ArticlePubMed
- 20. Minagawa Y, Saito Y. Active social participation and mortality risk among older people in Japan: results from a nationally representative sample. Res Aging 2015;37(5):481-499ArticlePubMedPDF
- 21. Ishikawa Y, Kondo N, Kondo K, Saito T, Hayashi H, Kawachi I, et al. Social participation and mortality: does social position in civic groups matter? BMC Public Health 2016;16: 394ArticlePubMedPMCPDF
- 22. Lynch JW, Smith GD, Kaplan GA, House JS. Income inequality and mortality: importance to health of individual income, psychosocial environment, or material conditions. BMJ 2000;320(7243):1200-1204ArticlePubMedPMC
- 23. Lyyra TM, Heikkinen RL. Perceived social support and mortality in older people. J Gerontol B Psychol Sci Soc Sci 2006;61(3):S147-S152ArticlePubMed
- 24. Blazer DG. Social support and mortality in an elderly community population. Am J Epidemiol 1982;115(5):684-694PubMed
- 25. Pettigrew KE. Lay information provision in community settings: how community health nurses disseminate human services information to the elderly. Libr Q 2000;70(1):47-85Article
- 26. Young AF, Russell A, Powers JR. The sense of belonging to a neighbourhood: can it be measured and is it related to health and well being in older women? Soc Sci Med 2004;59(12):2627-2637ArticlePubMed
- 27. Guehne U, Luck T, Busse A, Angermeyer MC, Riedel-Heller SG. Mortality in individuals with mild cognitive impairment. Results of the Leipzig Longitudinal Study of the Aged (LEILA75+). Neuroepidemiology 2007;29(3-4):226-234ArticlePubMedPDF
- 28. Obisesan TO, Gillum RF. Cognitive function, social integration and mortality in a U.S. national cohort study of older adults. BMC Geriatr 2009;9: 33ArticlePubMedPMCPDF
- 29. Poulin MJ, Brown SL, Dillard AJ, Smith DM. Giving to others and the association between stress and mortality. Am J Public Health 2013;103(9):1649-1655ArticlePubMedPMC
- 30. Serper M, Patzer RE, Curtis LM, Smith SG, O’Conor R, Baker DW, et al. Health literacy, cognitive ability, and functional health status among older adults. Health Serv Res 2014;49(4):1249-1267ArticlePubMedPMC
- 31. Lin JS, O’Connor E, SeRossompeRossom RC, Perdue LA, Burda BU, Thompson M, et al. Screening for cognitive impairment in older adults: an evidence update for the U.S. Preventive Services Task Force. Rockville: Agency for Healthcare Research and Quality; 2013. Report No. 14-05198-EF-1
- 32. Gussekloo J, Westendorp RG, Remarque EJ, Lagaay AM, Heeren TJ, Knook DL. Impact of mild cognitive impairment on survival in very elderly people: cohort study. BMJ 1997;315(7115):1053-1054ArticlePubMedPMC
- 33. Latkin CA, Edwards C, Davey-Rothwell MA, Tobin KE. The relationship between social desirability bias and self-reports of health, substance use, and social network factors among urban substance users in Baltimore, Maryland. Addict Behav 2017;73: 133-136ArticlePubMedPMC
REFERENCES
Figure & Data
References
Citations

- Figure
- Related articles
-
- Impact of Physical Activity on the Association Between Unhealthy Adolescent Behaviors and Anxiety Among Korean Adolescents: A Cross-sectional Study
- Effect Modification of Kidney Function on the Non-linear Association Between Serum Calcium Levels and Cardiovascular Mortality in Korean Adults
- The Moderating Effect of Gender on the Relationship Between Self-neglect and Suicidal Ideation in Older Adults of Korea
- Mediating Effect of Cognitive Function on the Relationship Between Geriatric Oral Health and Quality of Life Among Korean Seniors
 KSPM
KSPM

 PubReader
PubReader ePub Link
ePub Link Cite
Cite